Highlights
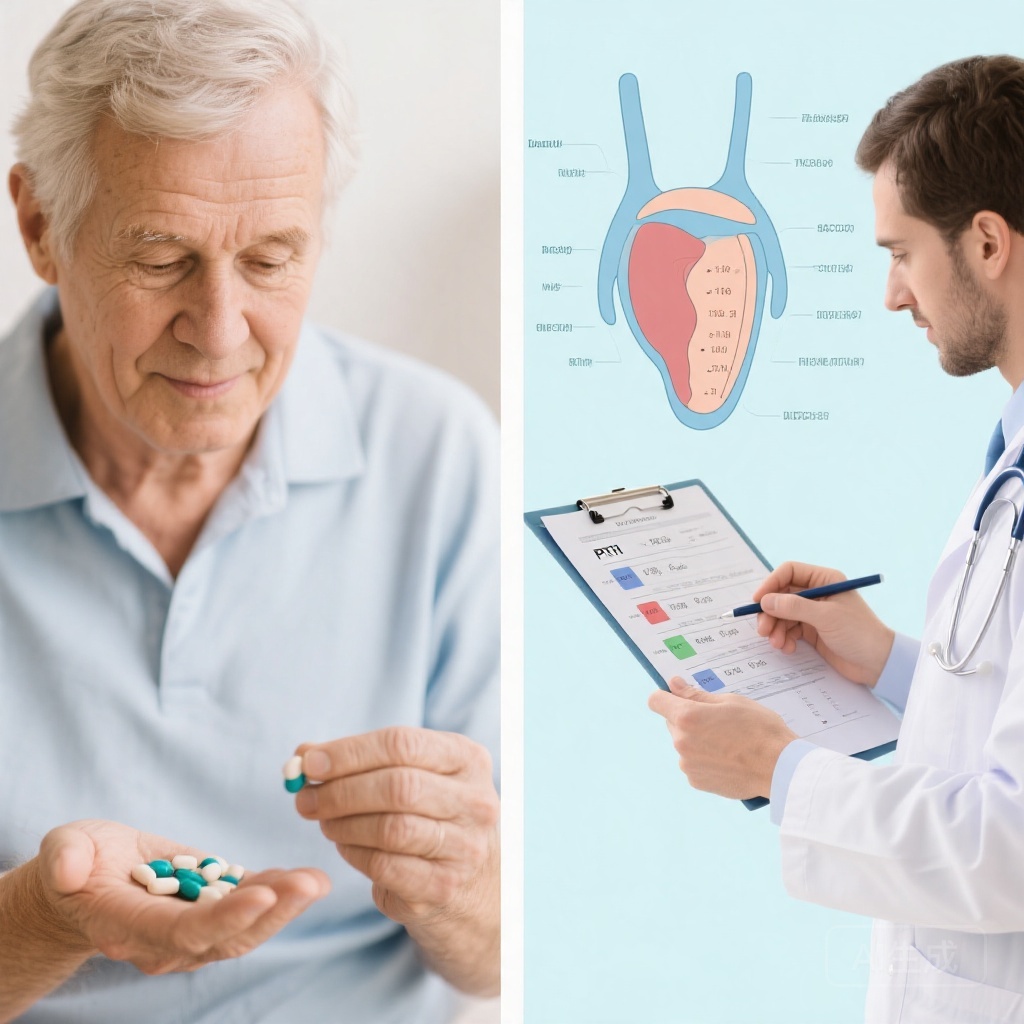
The study compared two calcium supplementation strategies after total thyroidectomy: routine prophylactic calcium with calcitriol (C+C) versus selective supplementation guided by 4-hour postoperative PTH levels.
No significant difference was found between groups in symptomatic hypocalcemia incidence (7.8% vs. 11.1%, P=0.36) or biochemical hypocalcemia (21.6% vs. 17.6%, P=0.53).
PTH-guided approach reduced unnecessary calcium supplementation without increasing adverse events or readmissions.
Findings support clinical equipoise—either strategy may be chosen based on institutional resources and protocols.
Background
Postoperative hypocalcemia remains the most common complication following total thyroidectomy, occurring in 10-35% of patients due to transient or permanent parathyroid gland dysfunction. While prophylactic calcium and vitamin D analogs have been standard practice, concerns about overtreatment (particularly in patients with preserved parathyroid function) have prompted investigation of biomarker-guided approaches. This multicenter trial addressed whether selective supplementation based on early postoperative PTH levels could maintain clinical outcomes while reducing unnecessary medication exposure.
Study Design
Population and Randomization
The pragmatic trial enrolled 258 adults undergoing total thyroidectomy for benign or malignant conditions across three tertiary hospitals (June 2022-July 2024). Patients with preexisting parathyroid disorders or prior parathyroid surgery were excluded. Participants were randomized to:
Interventions
1. PTH group (n=117): Supplemental calcium carbonate (3g/day) and calcitriol (0.5μg twice daily) initiated only if 4-hour postoperative PTH was <15 pg/mL (continued for 15 days)
2. C+C group (n=141): Routine prophylaxis with same calcium/calcitriol regimen for all patients (15 days)
Outcomes
Primary endpoint: Symptomatic hypocalcemia at 15 days (standardized symptom scale assessing perioral paresthesia, muscle cramps, etc.). Secondary outcomes included biochemical hypocalcemia (serum calcium <8.0 mg/dL), supplementation rates, adverse events, and readmissions.
Key Findings
Efficacy Outcomes
• Symptomatic hypocalcemia occurred in 9.3% overall (PTH group: 7.8% vs. C+C group: 11.1%; OR 0.68, 95% CI 0.29-1.57)
• Biochemical hypocalcemia (in subgroup with complete data): PTH 21.6% vs. C+C 17.6% (OR 1.29, 95% CI 0.57-2.93)
• No between-group differences in symptom severity or time to resolution
Resource Use and Safety
• PTH group required significantly less calcium supplementation (mean 7.2 vs. 15 days, P<0.001)
• Similar rates of hypercalcemia (2.6% vs. 3.5%), GI symptoms, and 30-day readmissions
• No differences across subgroups by age, malignant diagnosis, or surgeon volume
Expert Commentary
The equipoise demonstrated in this trial reflects evolving understanding of post-thyroidectomy parathyroid recovery dynamics. While PTH measurement adds marginal cost, selective supplementation may benefit healthcare systems by reducing cumulative medication exposure—particularly relevant given calcitriol’s narrow therapeutic index. The 15 pg/mL PTH cutoff aligns with prior observational studies, though some centers use higher thresholds (20-25 pg/mL) for supplementation triggers.
Conclusions
This level I evidence confirms that selective calcium supplementation based on early PTH assessment is non-inferior to routine prophylaxis for preventing post-thyroidectomy hypocalcemia. Clinicians may choose either strategy based on institutional resources, with PTH-guided approaches offering particular advantages in settings where medication cost or monitoring burdens are concerns. Future research should evaluate longer-term outcomes and cost-effectiveness across healthcare systems.
Trial Registration
ClinicalTrials.gov Identifier: NCT05252884
References
1. Garcia-Lozano C, et al. JAMA Otolaryngol Head Neck Surg. 2026;152(4):392-399. PMID: 41712216
2. Edafe O, et al. Br J Surg. 2021;108(10):1171-1179. PMID: 34265091 (PTH threshold meta-analysis)
3. AAES Guidelines for Post-Thyroidectomy Management (2025 update)