Background: The Unmet Need in Cardiac Resynchronization Therapy
Heart failure with reduced ejection fraction (HFrEF) remains a leading cause of cardiovascular morbidity and mortality worldwide. Among patients with HFrEF, those exhibiting left bundle-branch block (LBBB) demonstrate particular electrical dyssynchrony, contributing to ventricular remodeling, reduced cardiac output, and worse clinical outcomes. Cardiac resynchronization therapy (CRT) has become a cornerstone treatment for selected patients with HFrEF and conduction abnormalities, traditionally delivered through biventricular pacing (BiVP). However, despite technological advances, a substantial proportion of patients fail to achieve adequate response to BiVP, highlighting the need for alternative pacing strategies.
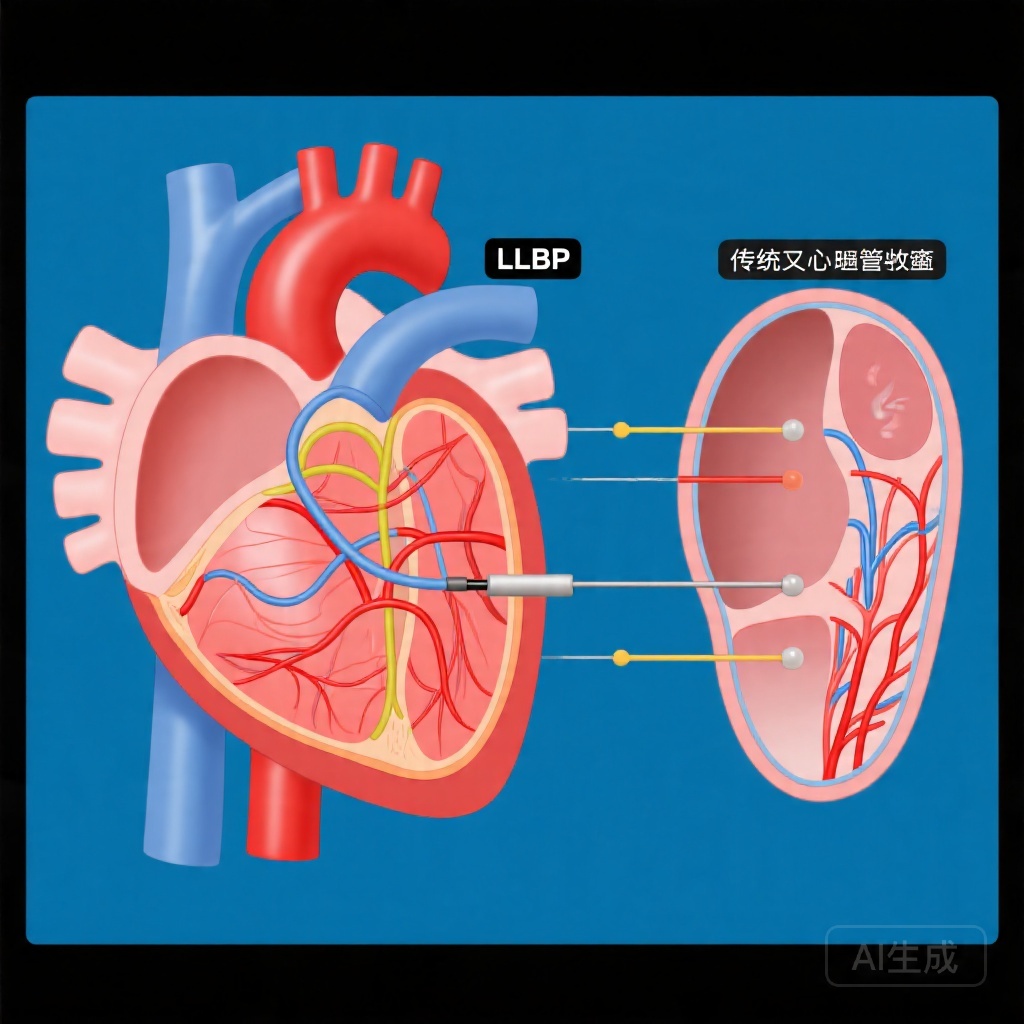
Left bundle-branch pacing (LBBP) has emerged as a novel physiological pacing approach that directly captures the left bundle branch system, potentially providing more synchronized ventricular activation than conventional BiVP. Early observational studies suggested favorable outcomes with LBBP, but robust evidence from randomized controlled trials has been limited. The HeartSync-LBBP trial addresses this critical evidence gap by prospectively comparing long-term clinical outcomes between LBBP and BiVP in patients with HFrEF and LBBB.
Study Design and Population
The HeartSync-LBBP trial was a multicenter, prospective, randomized clinical trial conducted across six centers in China. The study enrolled 200 patients meeting inclusion criteria of left ventricular ejection fraction (LVEF) of 35% or less and documented LBBB from October 2020 through March 2022, with follow-up continuing until September 2024. Analysis was performed from September to December 2024.
Patients were randomly assigned in a 1:1 ratio to receive either LBBP (n=100) or BiVP (n=100). The primary endpoint assessed time to the composite of death from any cause or heart failure hospitalization (HFH). Secondary endpoints included all-cause mortality alone, HFH as an individual component, echocardiographic response defined as an absolute increase in LVEF of 5% or greater, and super-response characterized by an absolute LVEF increase of 15% or improvement to an LVEF of 50% or higher.
The population included 136 male and 64 female participants. Procedural success rates were high in both groups, achieving 98% in the LBBP arm and 94% in the BiVP arm (P=0.28), indicating that LBBP can be implemented with comparable feasibility to conventional approaches. The median follow-up duration was 36 months, with an interquartile range of 33 to 39 months, providing meaningful long-term outcome data.
Primary Outcomes: Superiority of LBBP
The HeartSync-LBBP trial demonstrated a statistically significant and clinically meaningful superiority of LBBP over BiVP for the primary composite endpoint. Among patients randomized to LBBP, only 8% experienced the primary outcome of death or heart failure hospitalization, compared to 28% in the BiVP group. This translated to a hazard ratio (HR) of 0.26 (95% confidence interval [CI], 0.12-0.57; P<0.001), representing a 74% relative risk reduction with LBBP.
This magnitude of benefit substantially exceeds what has been observed in many prior CRT studies and suggests that direct capture of the left conduction system may provide superior electrical resynchronization compared to coronary sinus-based left ventricular pacing. The confidence interval's upper boundary of 0.57 indicates robust statistical significance, and the narrow range suggests precise estimation of the treatment effect.
Secondary Outcomes: Disentangling the Components
Analysis of the individual components of the primary endpoint revealed important insights. While all-cause mortality showed a trend toward reduction with LBBP (2.0% vs 5.0%), this difference did not reach statistical significance (HR, 0.40; 95% CI, 0.08-2.04; P=0.25). The relatively low overall mortality rate during follow-up may have limited statistical power to detect differences in this hard endpoint.
In contrast, heart failure hospitalization demonstrated highly significant superiority of LBBP. The HFH rate was 7.0% in the LBBP group compared to 28.0% in the BiVP group, yielding a hazard ratio of 0.23 (95% CI, 0.10-0.52; P<0.001). This 77% reduction in hospitalization risk has substantial implications for patient quality of life, healthcare resource utilization, and healthcare costs. Heart failure hospitalizations represent devastating events for patients and represent a major driver of the economic burden associated with HFrEF.
Echocardiographic Response and Super-Response Rates
Echocardiographic assessment revealed similar overall response rates between groups. The proportion of patients achieving at least a 5% absolute increase in LVEF was 86% in the LBBP group and 81% in the BiVP group (P=0.34). Both rates are notably higher than historical CRT response rates, potentially reflecting the rigorous patient selection criteria requiring LBBB, which represents a patient population with greater likelihood of electrical resynchronization benefit.
However, when examining super-response—an especially desirable outcome characterized by dramatic improvement—LBBP demonstrated significant superiority. The super-response rate was 55% with LBBP compared to 36% with BiVP (P<0.007). Super-responders experience normalization or near-normalization of left ventricular function, representing the optimal therapeutic goal in CRT. The 19-percentage point absolute difference favoring LBBP suggests that direct conduction system pacing achieves more physiological ventricular activation, translating to superior structural reverse remodeling.
Clinical Implications and Expert Commentary
The HeartSync-LBBP trial represents a landmark investigation in the field of cardiac resynchronization therapy. The findings challenge the paradigm that BiVP represents the optimal approach for delivering CRT and suggest that conduction system pacing may emerge as the preferred strategy for suitable candidates with LBBB.
From a mechanistic perspective, LBBP achieves ventricular resynchronization by directly stimulating the left bundle branch, resulting in rapid, synchronized activation of the left ventricle via the native conduction system. This contrasts with BiVP, which delivers pacing impulses from the right ventricle and a coronary sinus tributary, potentially activating the left ventricle through less physiological pathways. The superior super-response rates with LBBP provide indirect evidence supporting this mechanistic advantage.
The high procedural success rate of 98% with LBBP, comparable to BiVP, is reassuring and suggests that conduction system pacing can be reliably performed in clinical practice, contingent upon appropriate operator training and expertise. However, it should be noted that LBBP requires specific technical skills and fluoroscopic landmarks, and the learning curve may be steeper than conventional RV pacing.
Several limitations merit consideration when interpreting these results. The trial was conducted exclusively in China, and whether these findings generalize to more diverse populations with different ethnicities, healthcare systems, and standard-of-care practices requires further investigation. The sample size of 200 patients, while appropriate for detecting the large effect sizes observed, limits the precision of estimates for less common outcomes. Additionally, the relatively short median follow-up of 36 months, while providing meaningful long-term data, may not capture very long-term effects or complications.
Future Directions and Research Gaps
The HeartSync-LBBP trial opens several important avenues for future research. Multicenter trials in North American and European populations would enhance generalizability. Comparative studies in broader heart failure populations, including those without LBBB or with milder LVEF reduction, would clarify the optimal patient selection criteria for LBBP. Cost-effectiveness analyses comparing LBBP and BiVP would inform healthcare policy decisions, particularly if LBBP can be demonstrated to reduce downstream costs through fewer hospitalizations and improved outcomes.
The durability of LBBP leads over extended periods also requires investigation, as lead performance over 10-15 years remains unknown. Registry data and post-marketing surveillance will be essential for capturing rare adverse events and long-term safety signals.
Conclusion
The HeartSync-LBBP randomized clinical trial provides compelling evidence that left bundle-branch pacing is superior to biventricular pacing for reducing the composite of death or heart failure hospitalization in patients with reduced ejection fraction and left bundle-branch block. At 3-year follow-up, LBBP achieved a 74% reduction in the primary endpoint, driven primarily by a 77% reduction in heart failure hospitalizations, alongside significantly higher super-response rates. These findings have the potential to reshape the landscape of cardiac resynchronization therapy, positioning conduction system pacing as the preferred approach for eligible patients. Further trials in diverse populations and healthcare settings are warranted to confirm and extend these promising findings.
Trial Registration
Chinese Clinical Trial Registry: ChiCTR2000036554
Reference
Chen X, Liu X, Li R, Wang Z, Liang Y, Zhang L, Wang W, Bai J, Wang J, Qin S, Zhang W, Yao T, Huang D, Chen T, Zhao X, Liao D, Li J, Mao J, Chelu MG, Su Y, Ellenbogen KA, Ge J. Long-Term Outcomes of Left Bundle-Branch Pacing vs Biventricular Pacing in Heart Failure: The HeartSync-LBBP Randomized Clinical Trial. JAMA cardiology. 2026 Apr 1;11(4):352-359. PMID: 41811342.