Highlights
• Proximal hypoglossal nerve stimulation (pHGNS) achieved >50% improvement in apnea-hypopnea index (AHI) in 58.2% of treated patients versus 13.5% in controls.
• Oxygen desaturation index (ODI) reduction ≥25% occurred in 68.7% of pHGNS patients versus 37.8% of controls.
• Significant improvement in Epworth Sleepiness Scale (ESS) scores was observed in the treatment group.
• No serious procedure-related adverse events were reported.
Background
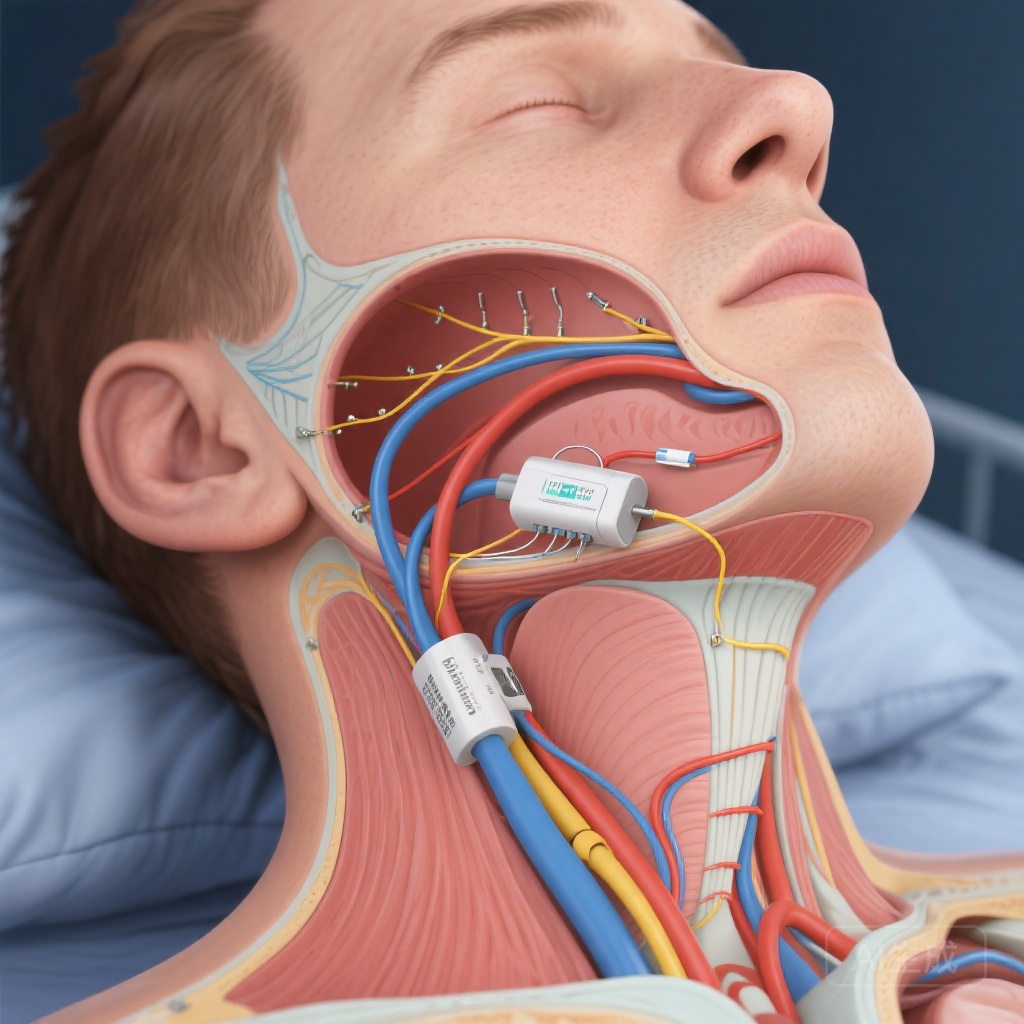
Obstructive sleep apnea (OSA) affects millions worldwide, with significant cardiovascular and neurocognitive consequences. While positive airway pressure (PAP) therapy remains first-line treatment, adherence rates remain suboptimal due to comfort and tolerance issues. Hypoglossal nerve stimulation (HGNS) has emerged as an alternative, but traditional approaches targeting distal nerve branches present technical challenges. The OSPREY trial investigated proximal HGNS (pHGNS), which stimulates multiple nerve branches closer to the main trunk, potentially offering both anatomical and functional advantages.
Study Design
The OSPREY study was a 7-month randomized controlled trial with a 6-month open-label extension conducted across 23 U.S. centers. Researchers enrolled 104 adults (mean age 55.6 years) with moderate-to-severe OSA (AHI 15-65 events/h) who were intolerant of PAP therapy. All participants underwent pHGNS device implantation at baseline, followed by 2:1 randomization to immediate treatment (month 1) or delayed treatment (month 7). The multicontact electrode system targeted proximal hypoglossal nerve branches rather than distal branches as in conventional HGNS.
Key Findings
The primary endpoint – proportion achieving >50% AHI improvement and AHI <20 events/h at 7 months – was met by 58.2% (95% CI 45.5-70.2%) of treated participants versus 13.5% (4.5-28.8%) of controls (p<0.001). Secondary outcomes showed:
• Oxygen desaturation index (ODI) reduced by ≥25% in 68.7% of treated patients versus 37.8% controls
• Median ESS improved from 10.0 to 6.0 in the treatment group (p<0.001) versus no change in controls
• Mean AHI decreased from 35.7 to 16.3 events/h in the treatment group
• Safety profile was favorable with no serious device-related adverse events
Expert Commentary
The OSPREY results suggest pHGNS may offer technical and clinical advantages over traditional HGNS. The proximal approach appears particularly effective due to:
• Broader neuromuscular activation from stimulating multiple nerve branches
• Potentially simpler surgical placement requiring less nerve dissection
• More consistent responder rates compared to distal HGNS literature
While promising, study limitations include lack of blinding and relatively short follow-up. Longer-term data from the open-label extension will be crucial for assessing maintenance of effect.
Conclusion
pHGNS demonstrates clinically meaningful benefits for moderate-to-severe OSA patients intolerant to PAP therapy, with nearly three-quarters achieving significant AHI or ODI improvements. These findings position pHGNS as a viable therapeutic option within the OSA treatment algorithm. Future research should compare pHGNS directly with traditional HGNS approaches and evaluate cost-effectiveness.
Funding and Registration
The study was funded by LivaNova PLC and registered at ClinicalTrials.gov (NCT04950894).