Highlights
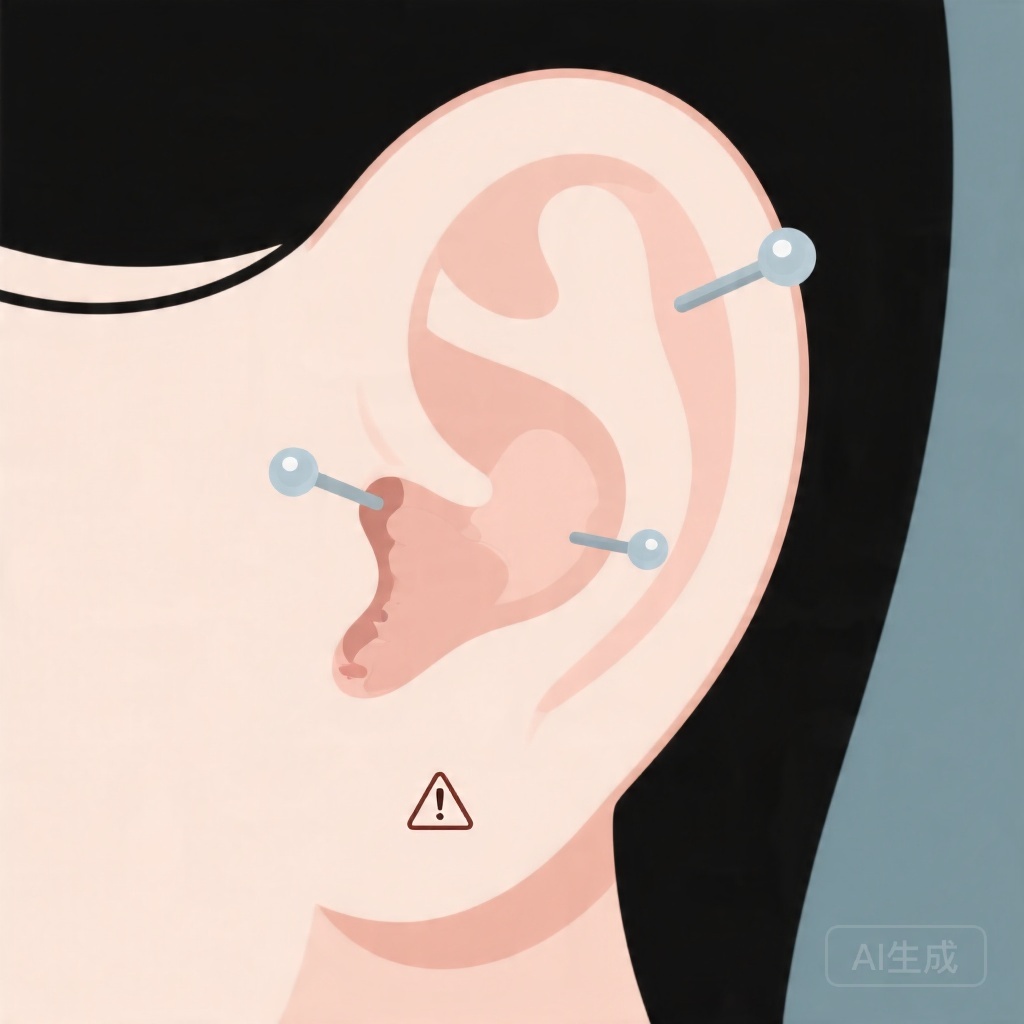
In a large anonymous survey of 3,270 adults reporting 9,016 ear piercings, auricular cartilage piercings were associated with a substantially higher overall complication rate than lobule piercings.
Complications occurred in 40.2% of cartilage piercings compared with 25.4% of lobule piercings, and infection was also more common in cartilage piercings.
Cartilage location and the occurrence of any complication both independently predicted piercing removal, suggesting that adverse events often have practical consequences, not merely cosmetic ones.
The findings support more explicit counseling about risk before cartilage piercing, especially when the piercing is elective and performed outside a medical setting.
Background
Ear piercing is common across age groups and cultures, and for most people it is a minor elective procedure. However, complications are not rare, and the clinical consequences can range from local pain, bleeding, and irritation to infection, scarring, keloid formation, and eventual loss of the piercing. The anatomical site matters. The earlobe is composed largely of soft tissue and has a richer blood supply, while auricular cartilage is relatively avascular and more vulnerable to delayed healing and infection-related injury.
From a clinical perspective, cartilage piercings deserve special attention because infections in cartilage can be more difficult to treat and may lead to deformity if not recognized promptly. In ENT practice, these infections can evolve into perichondritis or chondritis, conditions that may threaten the contour of the pinna. Despite these concerns, the comparative risk of complications between cartilage and lobule piercings has not always been clearly quantified in large populations.
This study addresses that gap by examining self-reported outcomes from a large adult cohort, with the goal of comparing complication and removal rates between cartilage and lobule piercings. Although survey-based data have inherent limitations, they can still provide useful real-world estimates and help inform shared decision-making.
Study Design
This was an anonymous electronic survey distributed to individuals with a University of Iowa email address. Respondents reported demographic information, the site of each ear piercing, age at piercing, piercing technique, who performed the piercing, and specific complications. The analysis included 9,016 ear piercings from 3,270 respondents.
Of these piercings, 6,275 (69.6%) were lobule piercings and 2,741 (30.4%) were auricular cartilage piercings. Multivariate logistic regression was used to compare complication and removal rates between the two sites, allowing adjustment for measured covariates. The primary outcomes were any reported complication and piercing removal. Infection was also assessed as an important secondary outcome.
Key Findings
The headline result is straightforward: cartilage piercings had more complications than lobule piercings. Overall complications were reported in 40.2% of cartilage piercings compared with 25.4% of lobule piercings, corresponding to an odds ratio (OR) of 1.98 with p<0.0001. In practical terms, cartilage piercings had nearly double the odds of a complication relative to lobule piercings in this cohort.
Infection, one of the most clinically relevant outcomes, was also more common in cartilage piercings. The reported infection rate was 30.3% for cartilage versus 23.8% for lobule piercings, with an OR of 1.39 and p<0.0001. While the absolute difference in infection rates was smaller than the difference in overall complications, the finding is still important because infection in cartilage can have disproportionate consequences due to the anatomy of the pinna and the potential for cartilage damage.
Removal of the piercing was another important outcome. Both cartilage site and the presence of any complication independently predicted removal, with ORs of 1.62 (p<0.0001) and 12.82 (p<0.0001), respectively. This suggests two clinically meaningful points: first, cartilage piercings are more likely to be abandoned; and second, when complications occur, people are far more likely to remove the piercing.
The very large odds ratio for complication-related removal is intuitive. Once pain, swelling, discharge, or infection develop, the piercing often becomes unacceptable to the wearer. For clinicians, this matters because the desire to preserve a piercing may delay care-seeking, potentially worsening the outcome. Counseling should therefore include not only the likelihood of complications but also the possibility that a complication may end with removal and possible scarring.
Interpreting the effect sizes
The odds ratio of 1.98 for any complication indicates a strong association, but it should still be interpreted in context. Survey data do not prove causation, and self-report may overestimate or underestimate the true incidence. However, because the comparison was within the same general adult population and adjusted with multivariate regression, the signal is unlikely to be trivial. The absolute complication difference of about 15 percentage points is clinically meaningful for a procedure many people perceive as low risk.
The infection difference deserves nuanced interpretation. A reported infection rate above 20% in both groups is higher than what many clinicians would expect from formal medical records, which likely reflects the survey design, differences in participant recall, and broad interpretation of what constitutes infection. Some respondents may have classified prolonged redness, drainage, or irritation as infection. Even so, the consistent relative difference between cartilage and lobule sites still supports the same practical conclusion: cartilage is riskier.
What likely explains the higher risk in cartilage?
The biological plausibility is strong. Cartilage has limited blood supply, which can impair local immune response and slow healing. Piercing through cartilage also increases the chance of pressure necrosis, sustained inflammation, and infection spreading into poorly vascularized tissue. In contrast, the lobule is more forgiving anatomically and usually heals more reliably. These differences are well recognized in clinical otolaryngology and are consistent with the study’s findings.
Expert Commentary
This study is valuable because it examines a large number of real-world piercings rather than relying on small case series. The sample size strengthens confidence in the general direction of effect, and the use of multivariate analysis improves internal validity compared with a simple unadjusted comparison. For clinicians, the results provide a data-supported basis for pre-procedure counseling.
At the same time, several limitations should temper overinterpretation. First, the cohort came from individuals with a University of Iowa email address, which may not represent the general population in terms of age, education, geography, or piercing behavior. Second, the data were self-reported and anonymous, so misclassification is possible. Respondents may not remember the exact timing, technique, or details of each complication. Third, the survey design introduces selection bias: people with memorable complications may have been more likely to respond. Fourth, the study cannot fully account for differences in piercing device, aftercare, jewelry material, or prior skin conditions, all of which may influence outcomes.
Another important issue is outcome definition. “Complication” may encompass a wide range of events with different clinical significance, from transient irritation to true infection requiring treatment. Similarly, the term “infection” in a survey may not map cleanly to clinician-diagnosed infection. Therefore, the absolute event rates should be interpreted cautiously, even though the comparative signal is informative.
Despite these limitations, the study aligns with established clinical understanding. Cartilage piercings are already known to carry a higher risk of perichondritis and delayed healing. The present data add a large cohort estimate that strengthens counseling messages. From a public health perspective, the findings support targeted education for piercers, consumers, and primary care clinicians about site-specific risk.
For practice, the study suggests several reasonable steps. Individuals considering cartilage piercing should be counseled that the risk of complications is meaningfully higher than for a standard lobule piercing. They should be advised to seek piercing from experienced personnel using sterile technique and appropriate jewelry, and to monitor closely for redness, swelling, pain, or drainage. Clinicians should also be prepared to evaluate suspected cartilage infection promptly, because delayed treatment may increase the risk of deformity.
Clinical Implications
Although ear piercing is elective and often performed outside traditional healthcare settings, the medical consequences can still enter the clinical domain. Primary care clinicians, pediatricians, dermatologists, and otolaryngologists all encounter complications from piercings. This study supports a more explicit risk discussion before cartilage piercing, much like informed consent for other minor procedures.
For patients who strongly prefer cartilage piercing, counseling should emphasize that not all piercings are equivalent. Anatomy matters. A lobule piercing generally carries less risk than a cartilage piercing, and this difference should be communicated in plain language. Where appropriate, shared decision-making should include discussion of the potential need for treatment, removal, and the possibility of residual cosmetic change.
Conclusion
In this large adult survey cohort, auricular cartilage piercings were associated with significantly higher odds of complications, including infection, than lobule piercings. Cartilage site and complication occurrence also predicted piercing removal. While survey-based design limits precise incidence estimates, the comparative message is clear and clinically relevant: cartilage piercings are not simply “another ear piercing,” and they warrant more careful counseling, technique, and follow-up than soft tissue lobule piercings.
For clinicians and the public alike, the take-home message is straightforward: if the goal is to minimize risk, the earlobe remains the safer option.
Funding and clinicaltrials.gov
The PubMed record provided for this article does not list funding details or a clinicaltrials.gov registration number. As a survey study, it may not have required prospective trial registration.
References
1. Ziegler JP, Pagedar NA, Moline M, Marcus K, Tanenbaum ZG, Hoffman HT, Owen SR. Ear Piercing Complications: Comparing Cartilage and Soft Tissue Piercings in a Large Survey Cohort. The Laryngoscope. 2026-04-17. PMID: 41998811.
2. Mayers D, et al. Complications of body piercing. Am Fam Physician. 2002;66(5):901-906.
3. Meltzer DI. Complications of body piercing. Am Fam Physician. 2005;72(10):2029-2034.
4. Brook I. Microbiology and management of perichondritis of the ear. J Laryngol Otol. 2002;116(4):252-255.
5. Centers for Disease Control and Prevention. Body Piercing and Tattoos. General public health information on infection prevention and safe aftercare.