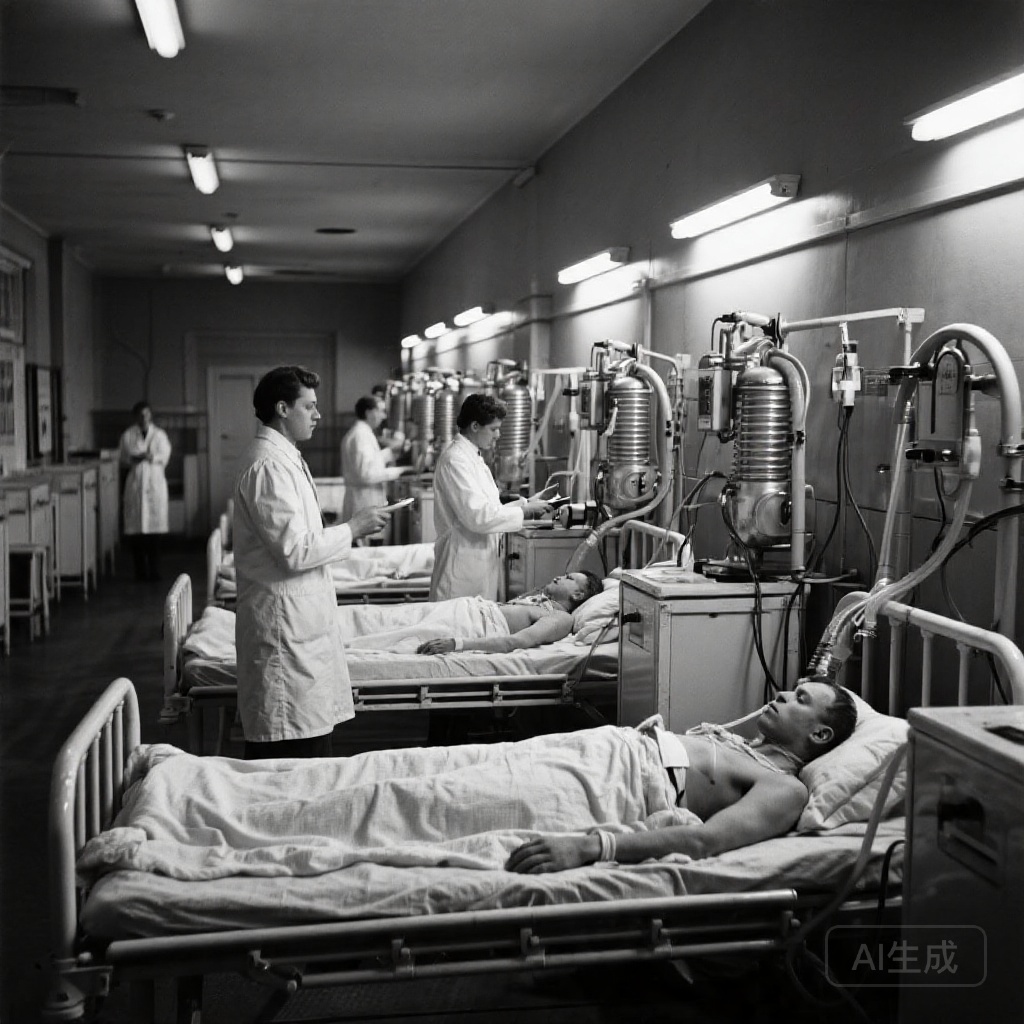
The Perfect Storm: Polio Strikes After Vaccine Dawn
In July 1955, just three months after Jonas Salk’s revolutionary polio vaccine received licensing, Massachusetts faced a devastating epidemic. This tragic timing created a unique crisis: While hope for prevention had finally emerged, thousands remained vulnerable to infection. The outbreak would become one of America’s last major polio epidemics, overwhelming Boston’s healthcare infrastructure as hospitals scrambled to accommodate paralyzed patients requiring respiratory support.
MGH’s Improvised War Zone
At Massachusetts General Hospital, the emergency response involved extraordinary delegation. Two assistant residents (equivalent to modern PGY-2 trainees) took charge of a rapidly assembled polio ward, while a second-year medical student established an adjacent laboratory. This setup became ground zero for both desperate patient care and unprecedented clinical research. The ward operated under crisis conditions, filled primarily with patients confined to iron lungs – mechanical respirators that encased entire bodies except the head.
Research Born at the Bedside
Despite 100-hour work weeks, these trainees conducted original patient-oriented studies literally steps away from the respirators. Their research focused on respiratory management nuances, fluid balance in paralyzed patients, and autonomic nervous system responses. The hospital’s preexisting culture of bedside investigation enabled this dual clinician-researcher role, while the era’s lack of formal consent requirements facilitated rapid data collection. Methodologically sophisticated for their time, these studies paralleled contemporary research on other diseases.
Boundaryless Medicine: The Double-Edged Sword
The absence of modern role boundaries allowed extraordinary clinical autonomy but raised ethical questions by today’s standards. Trainees made critical decisions without attending supervision, adjusted ventilator settings based on emerging research findings, and documented physiological responses without structured consent processes. This constant presence – what one resident described as “never more than 15 feet from the respirator” – enabled minute-by-minute observation that generated invaluable data on polio’s pathophysiology.
Contrasting Crises: Polio Versus Pandemic
This historical episode offers stark contrasts to trainee roles during COVID-19’s initial surge. While 1955 housestaff held frontline responsibility with wide decision-making latitude, modern trainees often faced restricted clinical roles despite pandemic needs. The divergence highlights how evolving concepts of supervision, liability, and structured training have reshaped medical education during crises.
Enduring Legacies
Evidence suggests this intense experience profoundly shaped participants’ careers, with many becoming leaders in pulmonary medicine, critical care, and infectious disease research. The polio ward’s hands-on translational research model – where bedside observations immediately informed treatment protocols – created a blueprint for clinician-scientist development that still influences academic medicine today.
Ethical Evolution in Medical Research
This historical analysis reveals how ethical frameworks have transformed since the 1950s. Contemporary requirements for institutional review, informed consent, and work-hour limits would have drastically altered these studies. The episode serves as both tribute to clinician dedication under extreme duress and reminder of medicine’s ongoing ethical maturation – balancing urgent knowledge needs against patient autonomy protections.