Background
Gastroesophageal reflux disease (GERD) remains a prevalent condition with significant morbidity and healthcare burden. Traditional diagnostic tools, such as endoscopy and ambulatory pH monitoring, have limitations in assessing mucosal integrity and predicting treatment response. Mucosal impedance (MI) emerges as a promising technique to address these gaps by directly measuring epithelial injury and barrier function.
Physiologic Rationale
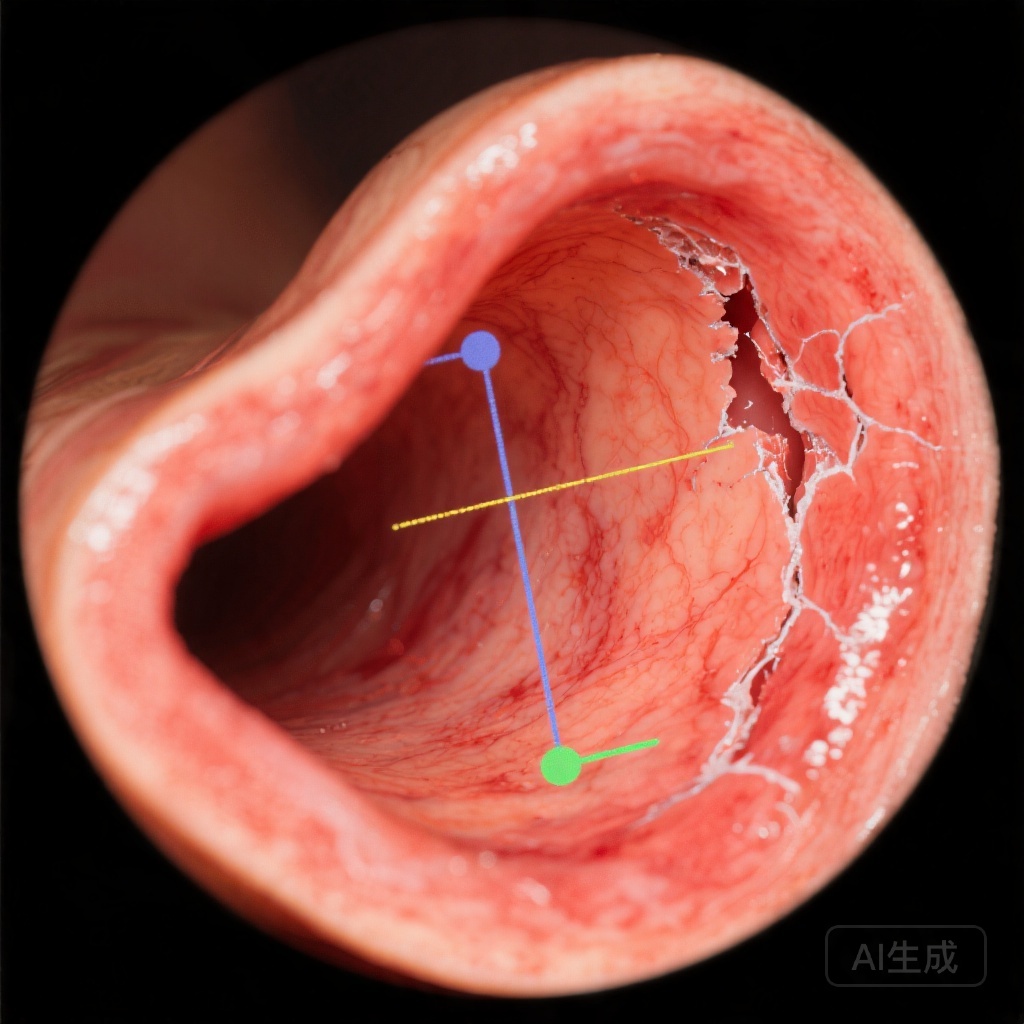
MI is an endoscopic measure that evaluates the electrical resistance of the esophageal mucosa, reflecting its structural integrity. Reduced impedance indicates mucosal damage from chronic acid exposure, even in non-erosive GERD. This provides a mechanistic link between reflux burden and symptom generation, beyond what pH monitoring alone can offer.
Technical Considerations
MI measurements are typically performed during endoscopy using specialized catheters. The procedure is minimally invasive and can be integrated into routine diagnostic workflows. Key technical aspects include standardization of measurement sites and avoidance of confounding factors like recent acid suppression therapy.
Clinical Evidence
Recent studies demonstrate that MI values are consistently lower in GERD patients compared to controls, with a strong correlation to symptom severity. Importantly, MI improves following effective medical or surgical therapy, suggesting its utility in monitoring treatment response. Data from surgical cohorts indicate that pre-operative MI may predict post-fundoplication outcomes, offering a potential tool for patient selection.
Implications for Surgical Management
MI provides objective criteria for identifying patients who may benefit most from anti-reflux surgery. By distinguishing between different GERD phenotypes, it helps tailor surgical approaches and set realistic expectations for symptom resolution. Post-operatively, MI can serve as a biomarker for assessing mucosal recovery and procedure success.
Expert Commentary
Leading gastroenterologists highlight MI’s potential to revolutionize GERD management by bridging the gap between functional testing and tissue-level pathology. However, they caution that larger, multicenter studies are needed to establish standardized protocols and validate its predictive value across diverse populations.
Conclusion
Mucosal impedance represents a paradigm shift in GERD diagnostics, offering a direct assessment of mucosal health that complements existing tools. Its integration into clinical practice could refine phenotyping, optimize treatment selection, and objectively evaluate therapeutic efficacy, particularly in surgical candidates.