Key Highlights
SGLT2 inhibitor therapy does not increase 1-year amputation risk in patients with diabetic foot ulcers, challenging prior concerns about potential harm. Patients receiving SGLT2 inhibitors demonstrated a dramatic reduction in 1-year mortality (1.1% vs 9.2%, P = 0.009), representing an 88% relative reduction in death risk. Wound healing time was significantly shorter in the SGLT2 inhibitor group, with a mean difference of 44 days (136.5 vs 181.2 days, P = 0.04). The findings provide important real-world evidence for the safety profile of these agents in a high-risk population.
Background
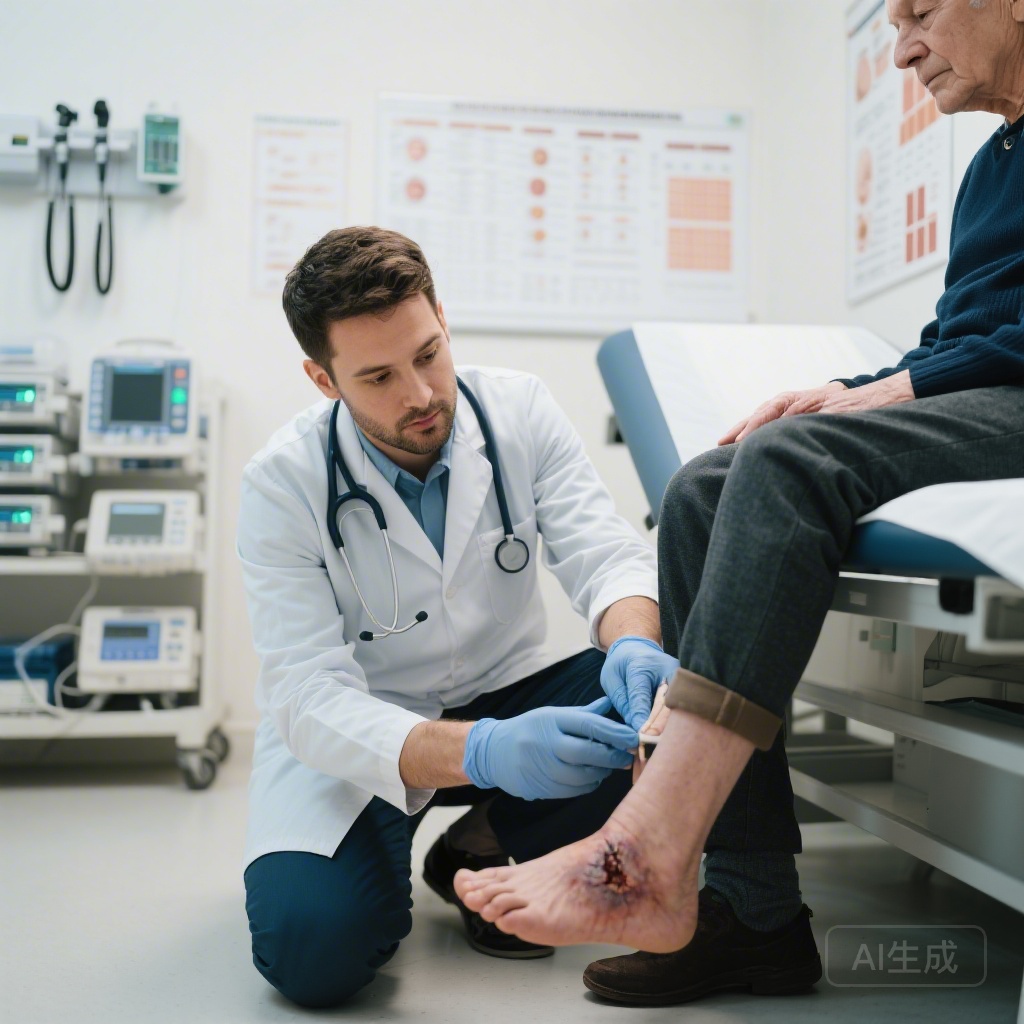
Diabetic foot ulcer (DFU) represents one of the most devastating complications of diabetes mellitus, serving as the leading cause of nontraumatic lower-limb amputation globally. The lifetime risk of developing a foot ulcer in patients with diabetes has been estimated at 19% to 34%, with approximately 20% of these wounds resulting in some form of amputation. Beyond the substantial morbidity associated with DFU, the economic burden is considerable, with healthcare costs for diabetic foot disease exceeding those of many common malignancies.
Sodium-glucose cotransporter 2 inhibitors (SGLT2is) have emerged as cornerstone therapies in type 2 diabetes management, demonstrating remarkable cardiovascular and renal benefits in large outcome trials. However, early signals from the EMPA-REG OUTCOME trial suggested a potential increase in lower-limb amputation risk with empagliflozin, generating substantial controversy and clinician concern. Subsequent analyses and other cardiovascular outcome trials have yielded inconsistent results, and the proportion of patients with active DFU in these trials remains largely unknown, limiting the applicability of these findings to real-world clinical practice.
The mechanistic basis for any potential amputation risk with SGLT2is has been the subject of considerable speculation. Proposed mechanisms include volume depletion leading to reduced tissue perfusion, increased hematocrit potentially promoting thrombosis, and accelerated wound catabolism. Despite extensive investigation, the clinical significance of these theoretical concerns in patients with established DFU has remained unclear.
The study by Dumortier and colleagues addresses this critical knowledge gap by specifically examining outcomes in patients with active diabetic foot ulcers receiving SGLT2 inhibitor therapy, providing highly relevant evidence for clinical decision-making in this high-risk population.
Study Design
This retrospective, monocentric study was conducted at a specialized diabetic foot center in France. The research team identified all patients treated for a new diabetic foot ulcer between January 2022 and May 2024 who had completed at least 1 year of follow-up. Patients were stratified into two groups based on SGLT2 inhibitor use at the time of DFU presentation: those receiving SGLT2i therapy (n = 94) and those not receiving these agents (n = 358).
The primary endpoint was the 1-year amputation rate, defined as any lower-limb amputation occurring within 12 months of DFU diagnosis. Secondary endpoints included 6-month wound healing rates, time to complete wound healing, and 1-year all-cause mortality. The study employed multivariable statistical modeling to adjust for potential confounders, including age, sex, diabetes duration, glycemic control, comorbidities, and ulcer characteristics.
The demographic characteristics of the study population reflected the typical profile of patients with diabetic foot disease: mean age of 70.2 ± 11.6 years, with 77% of participants being male. Cardiovascular comorbidities were prevalent in both groups, consistent with the established cardiovascular burden in this population.
Key Findings
Amputation Outcomes
The primary finding of this study provides reassuring evidence regarding the safety of SGLT2 inhibitors in patients with diabetic foot ulcers. In the adjusted statistical model, there was no significant association between 1-year amputation rate and SGLT2 inhibitor use (P = 0.688). This finding addresses the primary clinical concern that has limited SGLT2 inhibitor prescribing in patients with or at risk for foot ulcers.
The absence of an increased amputation risk is particularly notable given the theoretical concerns raised by earlier cardiovascular outcome trials. The specific focus on patients with established DFU, rather than general diabetes populations, provides direct evidence applicable to clinical practice in wound care settings.
Wound Healing
Analysis of wound healing outcomes revealed encouraging trends favoring the SGLT2 inhibitor group, though some results did not reach statistical significance. The 6-month healing rate showed a clinically meaningful difference between groups (54.4% vs 44.5%), with a P-value of 0.091 that approached but did not achieve conventional statistical significance. This trend warrants consideration given the relatively modest sample size in the SGLT2i group (n = 94).
Perhaps the most compelling healing-related finding was the significant reduction in time to complete wound healing. Patients treated with SGLT2 inhibitors achieved complete healing in a mean of 136.5 ± 97.8 days compared to 181.2 ± 159.8 days in the non-SGLT2i group, representing a mean difference of 44 days (P = 0.04). This 24% reduction in healing time has important implications for patient quality of life, healthcare resource utilization, and infection risk during the vulnerable wound-open period.
Mortality Outcomes
The mortality findings represent the most striking result of this study. The 1-year all-cause mortality rate was dramatically lower in the SGLT2i group compared to the non-SGLT2i group (1.1% vs 9.2%, P = 0.009). This 88% relative risk reduction in mortality translates to a number needed to treat of approximately 12 patients to prevent one death over one year.
While the observational nature of this study precludes causal inference, this mortality benefit is consistent with the cardiovascular protection demonstrated in large randomized trials of SGLT2 inhibitors. Patients with diabetic foot ulcers carry a particularly high cardiovascular risk, and any intervention that reduces mortality in this population addresses a critical unmet need. The magnitude of the mortality benefit observed in this study exceeds what might have been anticipated based on general diabetes populations, potentially reflecting synergistic effects in the high-risk DFU setting.
Safety Profile
The study findings support an overall favorable safety profile for SGLT2 inhibitors in the context of active diabetic foot ulcer management. No signal for increased amputation risk was detected, and no new safety concerns emerged. The mortality benefit, while requiring cautious interpretation given the study design, aligns with the established cardioprotective effects of this drug class.
Expert Commentary
The study by Dumortier and colleagues makes a valuable contribution to the growing body of evidence regarding SGLT2 inhibitor safety in diabetic foot disease. Several aspects merit careful consideration.
First, the retrospective, single-center design introduces inherent limitations. While the investigators employed multivariable adjustment to control for confounding, unmeasured variables may have influenced outcomes. The significant mortality difference, in particular, warrants scrutiny regarding potential selection bias: patients deemed appropriate for SGLT2 inhibitor therapy may have differed systematically from those not receiving these agents in ways not fully captured by adjustment models.
Second, the sample size, while adequate for the primary endpoint, limits the precision of subgroup analyses and secondary endpoint estimates. The 6-month healing rate approaching but not achieving significance (P = 0.091) illustrates this limitation; a larger cohort might clarify whether the observed numerical difference represents a true treatment effect.
Third, the generalizability of findings from a specialized French diabetic foot center to other clinical settings requires consideration. Referral patterns, baseline care quality, and population characteristics may differ across healthcare systems and geographic regions.
Mechanistically, several hypotheses might explain the observed benefits. SGLT2 inhibitors promote glycosuria, potentially reducing glucose availability to wound pathogens and limiting bacterial proliferation. The diuretic effect may enhance tissue oxygenation through improved microcirculation. Anti-inflammatory and anti-fibrotic properties demonstrated in preclinical models could promote granulation tissue formation. The cardiovascular and renal protective effects likely contribute to mortality reduction through multiple pathways.
Clinical implications of these findings suggest that SGLT2 inhibitor therapy should not be withheld from patients with diabetic foot ulcers based on amputation concerns alone. The potential mortality benefit, if confirmed in additional studies, could position SGLT2 inhibitors as agents with favorable risk-benefit profiles specifically in the DFU population.
Conclusion
This retrospective study of 452 patients with diabetic foot ulcers provides important clinical evidence that SGLT2 inhibitor use is not associated with increased amputation risk at 1 year. The significant reductions in mortality and healing time observed in SGLT2 inhibitor-treated patients suggest potential benefits that extend beyond glucose lowering in this high-risk population.
The findings challenge the notion that SGLT2 inhibitors should be avoided in patients with or at risk for diabetic foot disease. While the mortality benefit requires validation in larger, prospective studies, the absence of increased amputation risk provides immediate reassurance for clinical decision-making. These results should encourage clinicians to consider SGLT2 inhibitor therapy as part of comprehensive diabetes management in appropriate patients with diabetic foot ulcers, recognizing the cardiovascular and potential wound-healing benefits of this drug class.
Future research should focus on prospective, multicenter studies with larger sample sizes to confirm these findings, investigate optimal timing of SGLT2 inhibitor initiation relative to wound onset, and explore mechanisms underlying the observed healing and mortality benefits.
Funding and Study Registration
No specific funding information was provided in the source material. The study was conducted at a French specialized diabetic foot center. For complete study details, refer to the original publication in Diabetes Care.
References
1. Dumortier C, Aho Glele S, Rouland A, et al. Effects of Sodium-Glucose Cotransporter 2 Inhibitor Use on Mortality, Amputation, and Healing in Patients With Diabetic Foot Ulcer. Diabetes Care. 2026;49(4):674-681. PMID: 41739582.