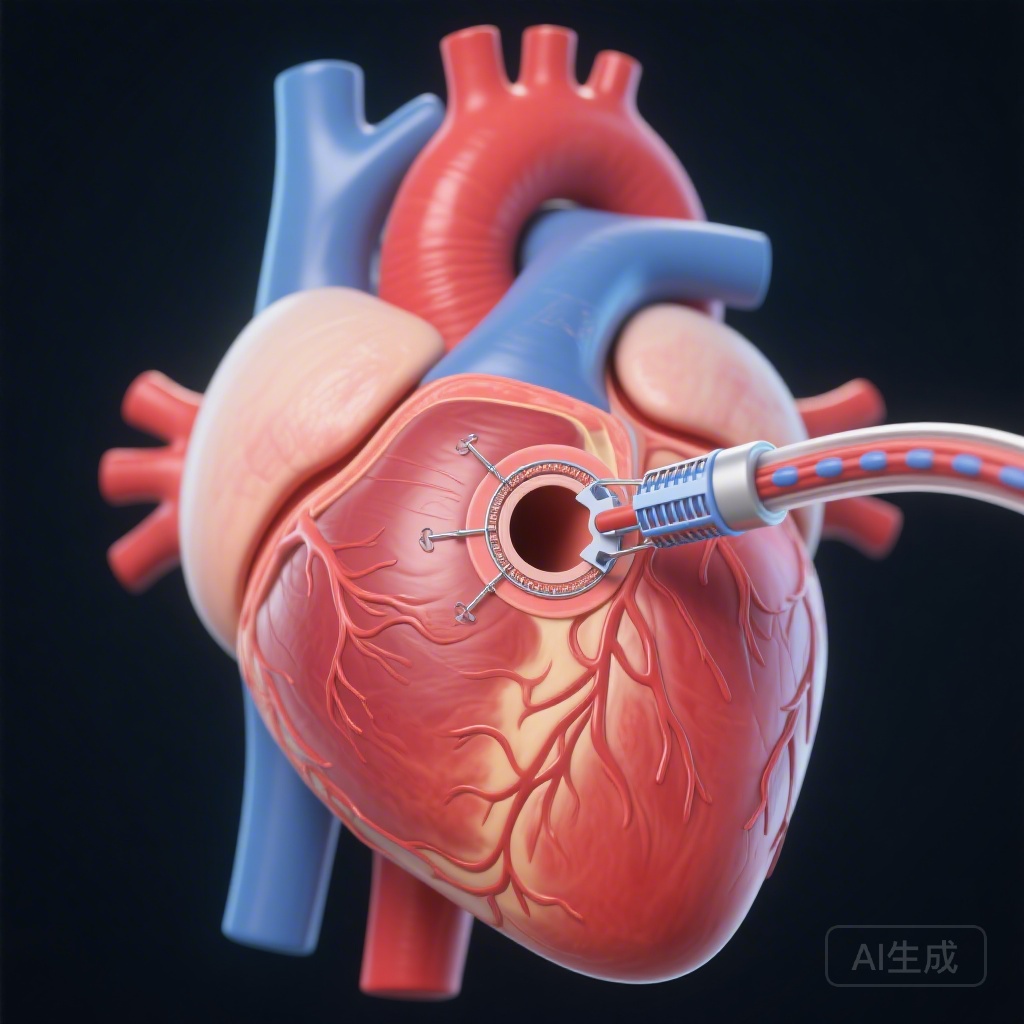
Patient Information
The study cohort comprised 130 consecutive patients who underwent transcatheter patent foramen ovale (PFO) closure between 2001 and 2006. The mean age of the participants was 46 years (SD: 14), with a near-equal distribution of gender (51.5% women, 48.5% men). All patients had a history of clinical events attributed to paradoxical embolism, including cryptogenic stroke, transient ischemic attack (TIA), or peripheral embolism. At the time of enrollment, none of the patients had other identifiable causes for their ischemic events, such as atrial fibrillation or significant carotid artery disease.
Diagnosis
The diagnosis for inclusion was PFO-associated paradoxical embolism. This was established through a rigorous diagnostic workup to exclude other sources of embolism. Key findings included the presence of a PFO confirmed via transesophageal echocardiography (TEE) with a bubble study demonstrating right-to-left shunting. The primary reasoning for diagnosis was the occurrence of an ischemic event (stroke or TIA) in the absence of traditional cardiovascular risk factors or alternative etiologies, commonly referred to as cryptogenic stroke.
Differential Diagnosis
During the initial evaluation, several alternative causes for the patients’ ischemic events were considered and ruled out:
- Atrial Fibrillation: Ruled out via electrocardiogram and prolonged cardiac monitoring.
- Carotid Artery Stenosis: Ruled out through Doppler ultrasound or MR angiography.
- Small Vessel Disease: Ruled out based on neuroimaging patterns.
- Prothrombotic States: While thrombophilia was present in a subset of patients (noted in 33% of those with recurrences), it was considered a contributing factor rather than the sole cause of the initial event.
Treatment and Management
All 130 patients underwent transcatheter PFO closure. The procedures were technically successful in 100% of the cases. Post-procedural management included echocardiographic follow-up within 1 to 6 months to ensure the stability of the device and the absence of significant residual shunts.
Following the procedure, patients were initially placed on antithrombotic therapy. However, the long-term management strategies evolved; over the 20-year follow-up period, 20.5% of the patients discontinued antithrombotic treatment entirely. The decision-making process for discontinuing therapy was based on individual clinical assessments and the absence of recurrent events or high-risk features.
Outcome and Prognosis
The 20-year follow-up provided robust data on the prognosis of PFO closure:
- Ischemic Recurrence: Recurrent events were remarkably low. Only 1 stroke (0.04 per 100 patient-years) and 6 TIAs (0.25 per 100 patient-years) were recorded over two decades.
- Mortality: 20 patients (15.3%) died during the follow-up period, with the vast majority (12.2%) due to non-cardiovascular causes, suggesting that the cardiac intervention did not negatively impact long-term survival.
- Safety: Bleeding events occurred in 13% of the cohort, with 6.9% classified as major. Notably, these events occurred exclusively in patients who remained on long-term antithrombotic therapy (17% vs 0% in those who discontinued; P = .04).
- Gender Disparity: Bleeding complications were significantly more frequent in women than in men (19.4% vs 6.3%; P = .03).
Discussion
This study represents one of the longest clinical follow-ups for PFO closure available in medical literature. The findings confirm that transcatheter PFO closure is a definitive and enduring therapy for preventing recurrent paradoxical embolism. The extremely low rate of recurrent stroke (less than 1% over 20 years) underscores the efficacy of the mechanical closure.
A critical takeaway from this case series is the relationship between long-term antithrombotic therapy and bleeding risk. Since no ischemic events occurred in the 20.5% of patients who stopped antithrombotics, the necessity of lifelong medication after successful PFO closure remains a point of clinical debate. This is particularly relevant for women, who showed a higher susceptibility to bleeding complications. Furthermore, the correlation between thrombophilia and recurrence (33% vs 4.8%) suggests that patients with known clotting disorders may require more vigilant monitoring or tailored pharmacological strategies.
In conclusion, while PFO closure provides excellent protection against stroke, clinicians must balance the long-term risks of antithrombotic therapy against the benefits, moving toward more personalized post-closure management plans.
References
Vidal-Calés P, Houde C, Battistolo Q, et al. Twenty-Year Follow-Up After Patent Foramen Ovale Closure in Patients With Paradoxical Embolism. JAMA Cardiology. Published online February 25, 2026. doi:10.1001/jamacardio.2025.41739488