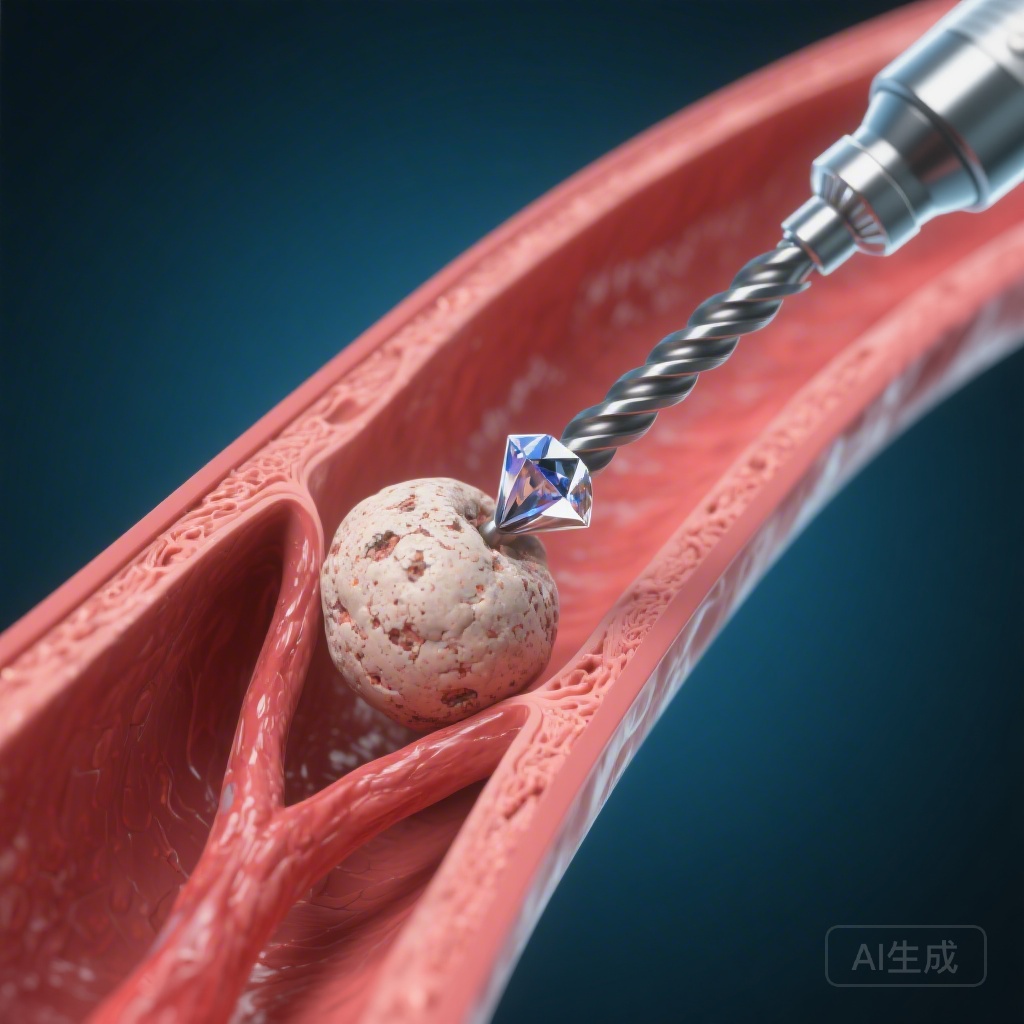
Introduction: The Clinical Challenge of Calcified Nodules
Calcified nodules (CNs) remain one of the most formidable challenges in interventional cardiology. Defined as protruding, eruptive masses of calcium that penetrate the internal elastic lamina and extend into the coronary lumen, CNs are a distinct phenotype from the more common circumferential or sheet-like calcification. Their presence is strongly associated with suboptimal stent expansion, stent eccentricity, and a significantly higher risk of target lesion revascularization (TLR) and stent thrombosis. While rotational atherectomy (RA) has long been the gold standard for modifying heavily calcified coronary lesions, its specific efficacy in treating CNs has remained a subject of debate. The recent publication of the U-SCAN registry substudy provides critical evidence that not all CNs are created equal, and the success of RA depends heavily on the surrounding vascular morphology.
Highlights
Rotational Atherectomy and TLR Risk
RA was independently associated with a 66% reduction in the risk of target lesion revascularization for patients with calcified nodules compared to conventional balloon angioplasty strategies.
The Role of Contralateral Calcification
The therapeutic benefit of RA was exclusively observed in lesions featuring contralateral calcification, showing a dramatic reduction in TLR rates (8.6% vs. 51.6%). In the absence of this feature, RA provided no significant advantage.
IVUS-Guided Precision
The study underscores the necessity of intravascular ultrasound (IVUS) to identify specific morphological features, such as CN length and lumen area stenosis, to guide the selection of debulking devices.
Background: The Unmet Need in Calcified Lesion Management
Interventionalists often find themselves in a clinical dilemma when encountering calcified nodules. Unlike concentric calcification, which can be cracked or fractured using high-pressure balloons or intravascular lithotripsy (IVL), CNs are focal, dense, and often resistant to displacement. Rotational atherectomy works via the principle of differential cutting, where a diamond-coated burr preferentially ablates inelastic tissue (calcium) while sparing elastic tissue. However, the efficacy of the burr depends on its ability to maintain contact with the calcium. This study addresses the unmet medical need for a stratified treatment algorithm for CNs based on high-resolution intravascular imaging.
Study Design: The U-SCAN Registry Analysis
The U-SCAN (Coronary Intravascular Ultrasound for Calcified Nodule) registry is a multicenter, retrospective study designed to evaluate the clinical outcomes of patients with IVUS-identified CNs. In this specific substudy, researchers analyzed 348 patients who underwent percutaneous coronary intervention (PCI). To ensure the integrity of the data, the investigators excluded patients with in-stent restenosis, those where alternative debulking devices (like orbital atherectomy or IVL) were used, cases where the device failed to pass, and those with poor IVUS image quality. The final cohort consisted of 209 patients, of whom 79 (37.8%) were treated with RA prior to stenting, while 130 (62.2%) were treated with conventional balloon-based strategies.
Key Findings and Results
The primary outcome of the study was the rate of target lesion revascularization (TLR) over a median follow-up period of 2.1 years. The researchers employed multivariable Cox proportional hazards models to adjust for confounding variables and identify independent predictors of clinical failure.
RA as an Independent Predictor
The RA group demonstrated a lower incidence of TLR compared to the non-RA group (25.3% vs. 31.5%). When adjusted for patient and lesion characteristics, RA emerged as a robust independent predictor of reduced TLR, with a hazard ratio (HR) of 0.34 (95% CI, 0.19-0.62; P < 0.001). This suggests that in the broad population of CN patients, RA offers a protective effect against future revascularization needs.
The Critical Impact of Contralateral Calcification
The most striking finding of the study was the interaction between RA and the presence of contralateral calcification (CC). Contralateral calcification refers to the presence of calcium on the vessel wall directly opposite the calcified nodule. In patients with CC, the TLR rate was remarkably lower in the RA group (8.6%) compared to the non-RA group (51.6%; P < 0.001). Conversely, in patients without CC, the TLR rate was actually higher in the RA group (38.6%) than in the non-RA group (25.3%), though this did not reach statistical significance (P = 0.11). The interaction P-value was highly significant (P < 0.001), indicating that the presence of CC is a mandatory prerequisite for RA efficacy in this patient population.
IVUS Morphological Predictors
Beyond the use of RA, the study identified several IVUS-derived parameters that correlated with a higher risk of TLR:
- Greater lumen area stenosis at the site of the nodule.
- Longer calcified nodule length.
- Smaller final minimum lumen area (MLA) after stenting.
- Adjacent circumferential calcification.
Expert Commentary: Mechanistic Insights and Clinical Implications
The clinical community has long suspected that the efficacy of rotational atherectomy is highly dependent on the “backboard” effect. When a diamond burr encounters a calcified nodule in a vessel where the opposite wall is soft and compliant, the burr tends to deflect away from the nodule, pushing the elastic tissue outward rather than ablating the hard calcium. This leads to “wire bias” issues and inadequate lesion modification.
However, when contralateral calcification is present, the vessel wall is rigid on both sides. This rigidity prevents the burr from deflecting, forcing it to maintain high-pressure contact with the calcified nodule. This leads to more effective ablation, a smoother lumen, and better subsequent stent expansion. These findings suggest that for CNs without contralateral calcification, alternative strategies—perhaps intravascular lithotripsy or focused balloon angioplasty—might be more appropriate than RA.
While the study provides powerful evidence, it is important to note its limitations. As a retrospective registry analysis, it is subject to selection bias. Furthermore, the study utilized IVUS rather than optical coherence tomography (OCT). While IVUS is excellent for assessing deep calcium and vessel dimensions, OCT provides superior resolution of the endoluminal surface and may offer more detail on the “eruptive” nature of the nodule.
Conclusion and Summary
The U-SCAN registry substudy represents a significant step forward in the precision management of complex coronary calcification. Rotational atherectomy is not a universal solution for all calcified nodules, but when applied to the right morphological substrate—specifically lesions with contralateral calcification—it offers a dramatic reduction in the risk of target lesion revascularization. Clinicians should prioritize pre-procedural intravascular imaging to map the calcium distribution, ensuring that debulking strategies are tailored to the specific mechanical environment of the coronary artery. This morphology-guided approach is likely to improve the long-term durability of PCI in our highest-risk patients.
Funding and Registration
This study was part of the U-SCAN registry. Clinical trial registration can be found at: https://jrct.mhlw.go.jp/; Unique identifier: jRCT1050240037.
References
Yabumoto N, Fujino M, Kiyoshige E, et al. Enhanced Efficacy of Rotational Atherectomy for Calcified Nodules With Contralateral Calcification: Insights From a Multicenter Intravascular Ultrasound Imaging Study. Circ Cardiovasc Interv. 2026 Feb 11:e015932. doi: 10.1161/CIRCINTERVENTIONS.125.015932.