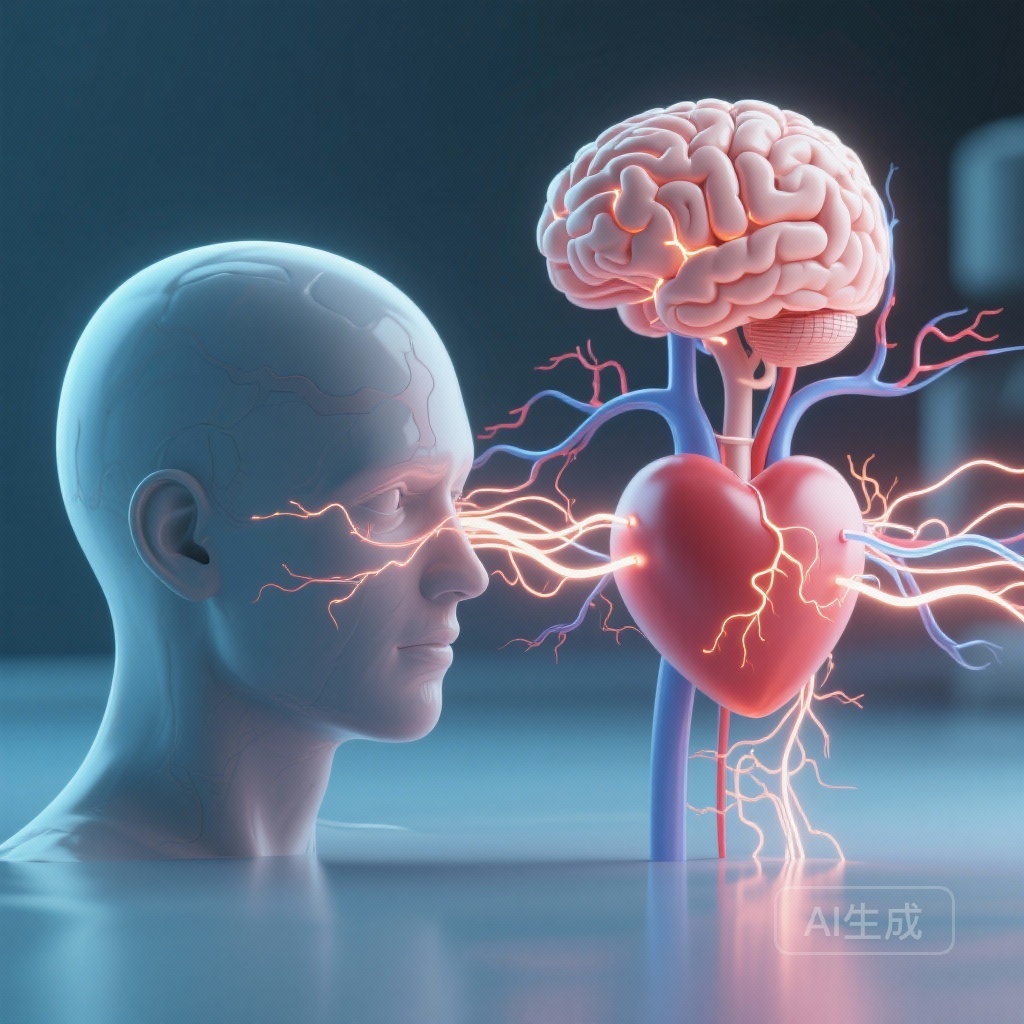
Introduction: The Unseen Drivers of Ischemic Heart Disease
For decades, the prevention of acute coronary syndrome (ACS) has focused predominantly on the ‘traditional’ risk factors: dyslipidemia, hypertension, diabetes mellitus, and tobacco use. While these factors remain the cornerstones of cardiovascular risk assessment, a significant portion of the global burden of heart disease remains unexplained or inadequately managed. Emerging evidence suggests that the mind-heart connection is not merely a psychological phenomenon but a clinical reality with profound physiological consequences. A landmark systematic review and meta-analysis published in JAMA Psychiatry by Gupta et al. (2026) provides a robust, evidence-based quantification of how mental disorders serve as potent precursors to ACS.
The Changing Landscape of ACS Risk Factors
Mental disorders are increasingly recognized as systemic conditions that influence multiple physiological pathways. However, until recently, the magnitude of their association with ACS was varied across different studies. The study by Gupta and colleagues addresses this gap by synthesizing data from over 22 million participants, offering a high-resolution view of the risk profile associated with depression, anxiety, PTSD, sleep disorders, and more severe psychiatric conditions like bipolar and psychotic disorders.
Study Design and Methodology
This systematic review and meta-analysis adhered to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) 2020 guidelines. The researchers conducted an exhaustive search of MEDLINE, Embase, and PubMed for studies published from inception through July 2025. The inclusion criteria were rigorous: observational or randomized studies that measured the association of any clinical mental disorder (diagnosed via DSM or ICD criteria) with incident ACS events, including myocardial infarction and unstable angina.
The quantitative synthesis utilized random-effects meta-analysis to account for heterogeneity across studies. To ensure the reliability of the findings, the researchers assessed study quality using the National Institutes of Health (NIH) Study Quality Assessment Tools and evaluated the evidence certainty using the Grading of Recommendations Assessment, Development, and Evaluation (GRADE) framework. The analysis included 25 full-text articles involving 22,048,504 participants, with a median age of 48 years and a majority male population (59.1%).
Key Findings: Quantifying the Mind-Heart Connection
The results of the meta-analysis reveal a stark and statistically significant correlation between several mental health conditions and the subsequent development of ACS. These findings underscore that psychiatric morbidity is not just a comorbid state but a significant risk factor in its own right.
The Potency of PTSD and Sleep Disturbances
Perhaps the most striking finding of the study was the magnitude of risk associated with Posttraumatic Stress Disorder (PTSD). Patients with PTSD exhibited a nearly three-fold increase in the risk of ACS (Hazard Ratio [HR], 2.73; 95% CI, 1.94-3.84; P < .001). This association was supported by moderate GRADE certainty, making it one of the most robust findings of the analysis. Sleep disorders also emerged as a major factor, with an HR of 1.60 (95% CI, 1.22-2.10; P < .001), suggesting that the quality and duration of rest are critical for vascular health.
Depression and Anxiety: Persistent Risks
Common mental disorders like depression and anxiety were also significantly associated with ACS. Anxiety disorders showed an HR of 1.63 (95% CI, 1.40-1.89; P < .001), while depressive disorders were associated with a 40% increased risk (HR, 1.40; 95% CI, 1.11-1.78; P = .01). Although the GRADE certainty for depression was rated as very low, the consistency of the association across studies remains a cause for clinical concern.
The Paradox of Psychotic and Bipolar Disorders
Interestingly, the study did not find a statistically significant association for bipolar disorder (HR, 1.48; 95% CI, 0.47-4.61) or psychotic disorders (HR, 0.97; 95% CI, 0.01-178.30). However, the researchers noted that the point estimates for bipolar disorder were similar to other mental health conditions, but the wide confidence intervals—likely due to smaller sample sizes or high variability in these specific cohorts—prevented reaching statistical significance. This highlights a need for further targeted research into these severe mental illnesses.
Expert Commentary: Mechanistic Insights
The biological plausibility linking mental health to ACS is well-established but multifaceted. Chronic stress, particularly in PTSD and anxiety, leads to the overactivation of the hypothalamic-pituitary-adrenal (HPA) axis and the sympathetic nervous system. This results in chronic elevations of cortisol and catecholamines, which in turn promote endothelial dysfunction, systemic inflammation (increased C-reactive protein and cytokines), and increased platelet reactivity—all of which are precursors to plaque rupture and coronary thrombosis.
Furthermore, sleep disorders contribute to cardiovascular strain through intermittent hypoxia, sympathetic surges, and metabolic disturbances that accelerate atherosclerosis. There is also a significant behavioral component: patients with mental disorders may face greater challenges with medication adherence, smoking cessation, and maintaining a healthy diet, creating a feedback loop of increasing cardiovascular risk.
Clinical Implications: A Call for Integrated Care
The findings of this meta-analysis have significant implications for both primary care and cardiology. First, mental health screening should be considered an essential component of cardiovascular risk assessment. Just as a clinician would monitor blood pressure or glucose levels, assessing for PTSD and sleep quality could provide a more accurate picture of a patient’s risk profile.
Second, the high HR for PTSD suggests that trauma-informed care is not just a psychological necessity but a cardiovascular intervention. Collaborative care models, where psychiatrists and cardiologists work together, may be the most effective way to address the complex needs of these patients. For the health policy expert, this data supports the allocation of resources toward mental health services as a means of reducing the long-term burden of ischemic heart disease on the healthcare system.
Conclusion: Bridging the Gap
This systematic review and meta-analysis confirm that mental disorders—especially PTSD and sleep disorders—are major independent risk factors for acute coronary syndrome. While the certainty of evidence varies, the overall trend is undeniable: the heart cannot be treated in isolation from the mind. Future research should focus on whether treating these mental disorders can directly reduce the incidence of ACS, potentially opening a new frontier in preventive cardiology.
References
Gupta A, Tejpal T, Seo C, et al. Mental Disorders as a Risk Factor of Acute Coronary Syndrome: A Systematic Review and Meta-Analysis. JAMA Psychiatry. 2026; doi:10.1001/jamapsychiatry.2025.4253.