Integrating Traditional Wisdom with Modern Cardiology: The MUTTON-HF Trial
The intersection of nutritional science and cardiovascular medicine has long recognized that diet is a cornerstone of heart failure (HF) management. However, standard dietary recommendations often fail to account for the social determinants of health, particularly nutrition insecurity, which disproportionately affects Indigenous communities in the United States. The MUTTON-HF (Medically Utilized Tailored Traditional Foods to Optimize Nutrition in Heart Failure) trial represents a paradigm shift in how clinicians approach HF care in these populations by leveraging the ‘Food is Medicine’ framework within a culturally grounded context.
Highlights
1. MUTTON-HF is the first pragmatic randomized controlled trial to evaluate the efficacy of an Indigenous culturally and medically tailored meal program for heart failure. 2. The study addresses nutrition insecurity by providing locally sourced Diné (Navajo) produce and meat, rather than generic low-sodium meals. 3. Primary endpoints focus on 90-day all-cause hospitalization and emergency department utilization, directly targeting the high readmission rates seen in rural tribal populations.
Background: The Burden of Nutrition Insecurity and Cardiovascular Disparity
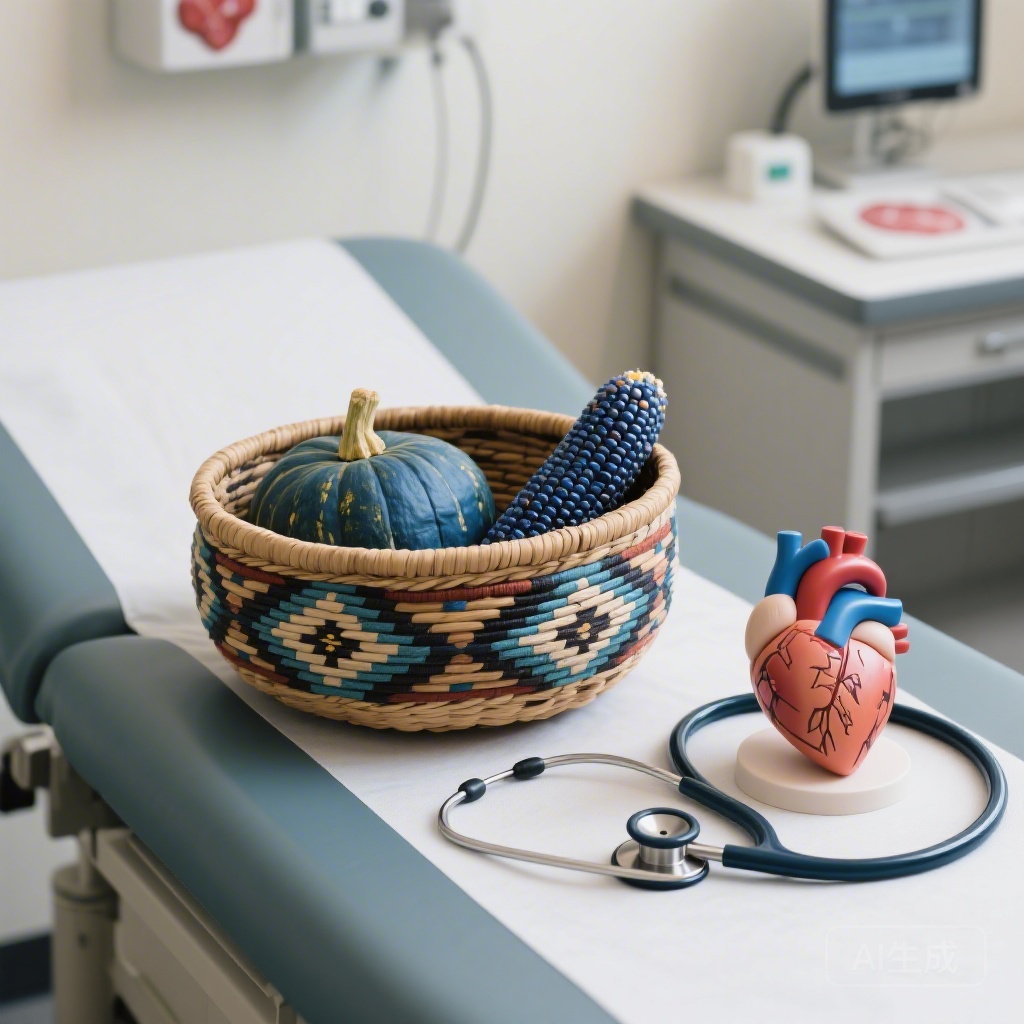
For the Diné (Navajo) people, cardiovascular disease remains a leading cause of morbidity and mortality. This disparity is not merely biological; it is rooted in historical and systemic factors that have led to the erosion of traditional food systems. Many tribal lands are classified as food deserts, where access to fresh, nutrient-dense produce is limited, and processed, high-sodium foods are more readily available. This nutrition insecurity is a potent driver of heart failure exacerbations, as poor diet quality leads to fluid overload, hypertension, and metabolic dysfunction.While medically tailored meals (MTMs) have shown promise in reducing hospitalizations in urban populations, they have rarely been adapted for rural Indigenous settings or designed around traditional pre-contact food systems. The MUTTON-HF study seeks to fill this gap by reclaiming traditional foods—such as blue corn, squash, and locally sourced mutton—as therapeutic interventions.
Study Design and Methodology
The MUTTON-HF trial is a 2-center, pragmatic, open-label randomized controlled trial (RCT) conducted at Indian Health Service (IHS) sites. The pragmatic design is intentional, ensuring that the results are generalizable to real-world clinical settings within tribal healthcare systems.
Patient Population and Stratification
The study aims to enroll 204 subjects who identify as Diné and have a confirmed diagnosis of heart failure. Eligibility requires a recent hospitalization or emergency room visit for HF within the last 12 months, identifying a high-risk cohort likely to benefit from intensive nutritional support. Randomization is performed in a 1:1 ratio, stratified by gender, age (under 65 vs. 65 and older), and left ventricular ejection fraction (LVEF <50% vs. ≥50%). This stratification ensures that the study can assess efficacy across the spectrum of heart failure, including both reduced and preserved ejection fractions.
The Intervention: Culturally and Medically Tailored Meals
The intervention group will receive culturally and medically tailored meals for 8 weeks. Unlike standard MTM programs, MUTTON-HF utilizes community-based participatory methods to ensure the meals are not only heart-healthy (low sodium, high fiber) but also culturally resonant. The meals incorporate traditional Diné recipes and ingredients sourced from local Native producers. The control group will receive ‘usual dietary advice,’ which typically consists of standard educational materials on sodium and fluid restriction.
Primary and Secondary Endpoints: A Multi-Dimensional Evaluation
The primary efficacy endpoint is the proportion of patients with at least one all-cause hospitalization or emergency room visit within 90 days of enrollment. This timeframe is critical, as the post-discharge period is the most vulnerable window for HF patients.
Secondary Clinical and Quality of Life Outcomes
Secondary outcomes are comprehensive, reflecting the holistic nature of the intervention:1. HF-Specific Utilization: Hospitalizations and ER visits specifically related to heart failure exacerbations. 2. Health-Related Quality of Life: Measured using the Kansas City Cardiomyopathy Questionnaire (KCCQ), a validated tool for assessing the symptomatic and functional impact of HF. 3. Nutritional and Socioeconomic Metrics: Measures of food insecurity, Indigenous nourishment, and financial strain. 4. Biological Markers: Changes in clinical biomarkers (such as NT-proBNP or inflammatory markers) from enrollment to the 8-week mark.
Expert Commentary: Scientific Plausibility and Clinical Significance
From a clinical perspective, the MUTTON-HF trial is significant because it moves beyond the ‘one-size-fits-all’ approach to medical nutrition. The biological plausibility of the intervention lies in the nutritional profile of traditional Indigenous diets, which are naturally high in complex carbohydrates, fiber, and phytochemicals, while being lower in the processed sugars and sodium prevalent in the modern Western diet.Furthermore, the psychological and social impact of cultural reclamation cannot be understated. For many Indigenous patients, the medical system can feel alienating. By integrating traditional foods, the MUTTON-HF intervention may improve patient engagement, treatment adherence, and overall trust in the healthcare system. This study serves as a critical test of whether addressing the social determinants of health through cultural assets can improve hard clinical outcomes.
Study Limitations and Considerations
As a pragmatic, open-label trial, blinding participants to their diet is impossible, which introduces the potential for a ‘placebo’ or ‘Hawthorne’ effect regarding self-reported quality of life. However, the use of hard clinical endpoints like hospitalizations mitigates this concern. Additionally, the 8-week duration is relatively short for long-term behavioral change, but it is sufficient to observe effects on acute readmission rates and biomarker stabilization.
Conclusion and Future Implications
The MUTTON-HF trial represents a landmark effort in Indigenous cardiovascular health. By combining the rigorous methodology of an RCT with the protective assets of Indigenous culture, it provides a blueprint for future ‘Food is Medicine’ initiatives. If successful, this study will provide the evidence base needed for policy changes, such as the reimbursement of culturally tailored meals by Medicaid or the Indian Health Service, ultimately transforming heart failure management for rural and tribal populations.
Funding and Registration
This study is registered at ClinicalTrials.gov (NCT06549699). Funding and support involve collaborative efforts within the Indian Health Service and academic partners dedicated to tribal health equity.
References
1. Eberly LA, George C, Sandman S, et al. MUTTON-HF: Rationale and Design of a Study of an Indigenous Food is Medicine Intervention. Circulation: Heart Failure. 2026;e014013. PMID: 41766529. 2. Heisler M, et al. The Role of Food Insecurity in Heart Failure Management. American Journal of Cardiology. 2023. 3. Berkowitz SA, et al. Medically Tailored Meals and Health Care Use: A Propensity Score-Matched Cohort Study. JAMA Internal Medicine. 2019.