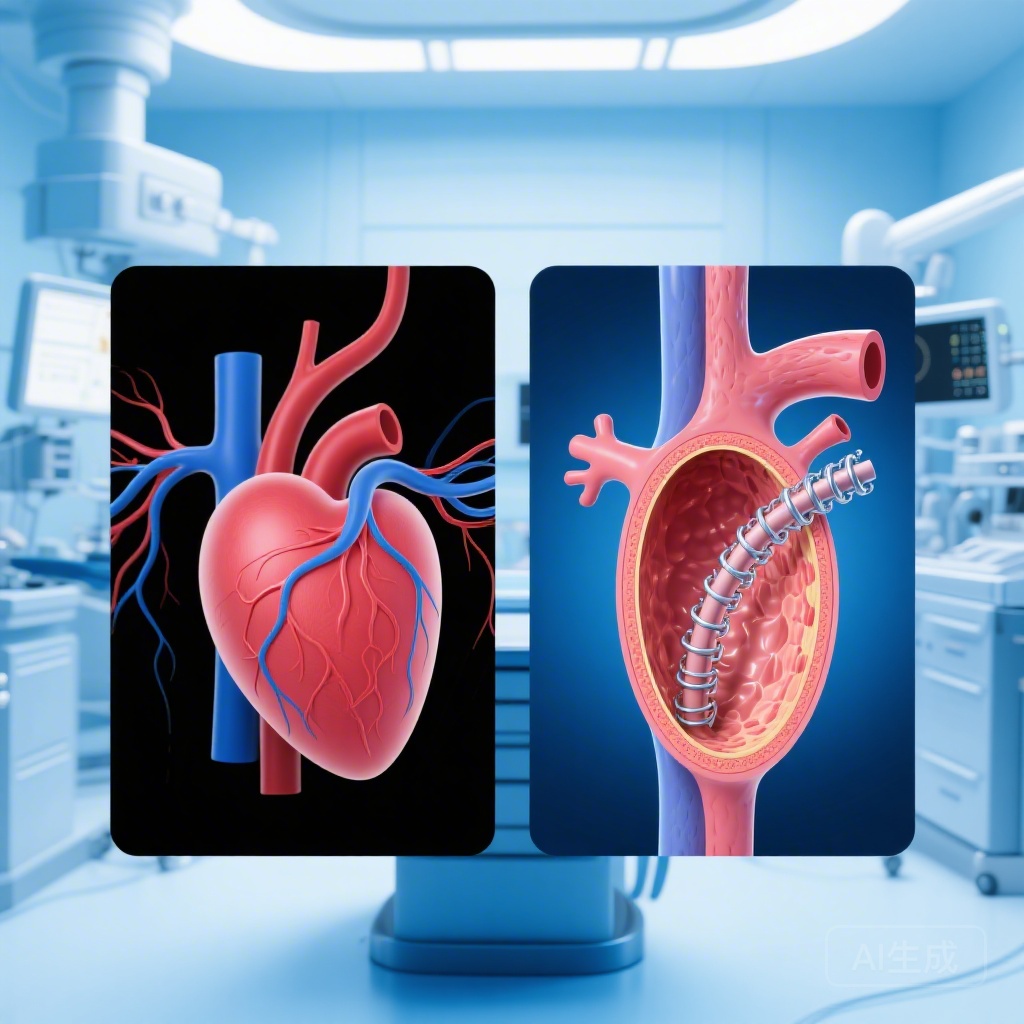
Introduction: The Shift from Seeing to Visualizing
For decades, coronary angiography has been the gold standard for guiding percutaneous coronary intervention (PCI). However, as a two-dimensional silhouette of a three-dimensional structure, angiography has inherent limitations, particularly in the assessment of complex coronary anatomy. The emergence of intravascular imaging—specifically Intravascular Ultrasound (IVUS) and Optical Coherence Tomography (OCT)—has allowed interventionalists to look within the vessel wall, providing precise measurements of vessel size, plaque morphology, and stent expansion. The RENOVATE-COMPLEX-PCI trial sought to determine if this enhanced visualization translates into long-term clinical benefits for patients with high-risk, complex lesions.
Highlighting Clinical Significance
The 5-year outcomes of the RENOVATE-COMPLEX-PCI trial provide several critical insights for the global cardiology community:
1. Intravascular imaging-guided PCI resulted in a 32% relative risk reduction in the primary composite endpoint of cardiac death, target vessel-related myocardial infarction (TV-MI), or clinically driven target vessel revascularization (TVR).
2. The clinical benefits were sustained over a median follow-up of 5.3 years, suggesting that the advantages of imaging-guided optimization are not merely periprocedural but offer long-term protection against late stent failure.
3. There was a notable reduction in the incidence of definite stent thrombosis, reinforcing the mechanistic role of imaging in ensuring optimal stent apposition and expansion.
The Burden of Complex Coronary Artery Disease
Complex coronary artery lesions—including bifurcations, chronic total occlusions (CTOs), long lesions, and left main disease—represent a significant proportion of modern PCI cases. These procedures carry a higher risk of complications, such as stent thrombosis, restenosis, and periprocedural myocardial infarction. While angiography can confirm the restoration of flow, it often fails to identify subtle but critical issues like edge dissections, malapposition, or under-expansion, which are the primary drivers of long-term failure in complex cases. As the patient population becomes older and more comorbid, the need for robust, evidence-based strategies to optimize these high-stakes interventions has never been greater.
Study Design and Methodology
The RENOVATE-COMPLEX-PCI trial was a prospective, multicenter, open-label, randomized superiority trial conducted across several high-volume centers in South Korea. The study enrolled 1,639 patients with complex coronary artery lesions. These patients were randomly assigned in a 2:1 ratio to receive either intravascular imaging-guided PCI (n=1,092) or traditional angiography-guided PCI (n=547).
Complex lesions were defined according to specific clinical and anatomical criteria, including true bifurcations, long lesions requiring multiple stents, left main disease, and severely calcified lesions. In the imaging group, the choice between IVUS and OCT was left to the operator’s discretion. The primary endpoint was a composite of major adverse cardiac events (MACE), specifically cardiac death, TV-MI, or clinically driven TVR. The trial was powered to detect a significant difference in these outcomes over a long-term follow-up period.
Key Findings: A Sustained Advantage
At a median follow-up of 5.3 years (interquartile range: 4.4-6.2 years), the primary endpoint occurred in 10.5% of patients in the imaging-guided group compared to 14.9% in the angiography-guided group. This difference was statistically significant (Hazard Ratio [HR]: 0.68; 95% Confidence Interval [CI]: 0.51-0.91; P = 0.009).
Secondary Outcomes and Component Analysis
The reduction in the primary endpoint was driven by lower rates across all individual components:
– Cardiac Death or TV-MI: 7.6% in the imaging group vs. 10.7% in the angiography group.
– Clinically Driven TVR: 4.4% in the imaging group vs. 6.2% in the angiography group.
– Definite Stent Thrombosis: A striking difference was observed, with only 0.1% (1 patient) in the imaging group compared to 0.7% (4 patients) in the angiography group.
Importantly, the safety profile was comparable between the two groups. There were no significant increases in procedure-related complications, such as contrast-induced nephropathy or coronary perforation, despite the additional steps required for intravascular imaging.
Mechanistic Insights: Why Imaging Succeeds
The clinical success of imaging-guided PCI in this trial can be attributed to several factors. First, imaging allows for more accurate vessel sizing, often leading to the selection of larger stents than angiography alone would suggest. Larger minimal stent areas (MSA) are strongly correlated with reduced rates of restenosis and thrombosis. Second, imaging identifies “geographic miss,” where a stent fails to cover the entire diseased segment. Third, the detection of edge dissections or severe malapposition allows for immediate corrective actions, such as further post-dilation or the placement of additional stents, before the patient leaves the lab.
Expert Commentary and Clinical Implications
For the clinical community, these results represent a call to action. While previous trials like ILUMIEN IV and ULTIMATE have shown the benefit of imaging, the 5-year data from RENOVATE-COMPLEX-PCI provide the long-term evidence needed to justify the routine use of IVUS or OCT in complex cases. Many experts argue that imaging should no longer be considered an “adjunct” but rather an essential component of the procedure.
However, challenges to widespread adoption remain. These include the increased cost of imaging catheters, the additional time required for image acquisition and interpretation, and the learning curve associated with mastering these technologies. Nevertheless, when considering the long-term cost-effectiveness—driven by the reduction in repeat revascularizations and hospitalizations for MI—the value proposition of imaging-guided PCI is compelling.
Recent guidelines from the European Society of Cardiology (ESC) and the American College of Cardiology/American Heart Association (ACC/AHA) have already begun to elevate the class of recommendation for intravascular imaging in specific scenarios. The RENOVATE-COMPLEX-PCI data will likely support a further push toward imaging as a Class I recommendation for all complex coronary interventions.
Conclusion
The 5-year outcomes of the RENOVATE-COMPLEX-PCI trial confirm that intravascular imaging is a transformative tool in the management of complex coronary artery disease. By significantly reducing the risk of cardiac death, myocardial infarction, and target vessel failure, imaging-guided PCI provides a superior clinical outcome that persists for years after the initial procedure. As interventional cardiology continues to evolve, the integration of these technologies will be paramount in achieving the highest standards of patient care and procedural success.
Funding and Trial Information
This study was supported by various research grants and conducted by the RENOVATE-COMPLEX-PCI Investigators. Trial registration: ClinicalTrials.gov (NCT03381872). The findings were published in the Journal of the American College of Cardiology (JACC).