Highlights
- A Phase 3, multi-center, pragmatic randomized controlled trial involving 220 participants found no significant difference in motor recovery between intensive task-specific training and usual rehabilitation care.
- The addition of 12 hours per week of intensive training for 10 weeks did not improve the International Standards for the Neurological Classification of SCI (ISNCSCI) Total Motor Score.
- Serious adverse events were low but present, including two deaths in the intervention group, highlighting the need for careful monitoring in subacute spinal cord injury (SCI) populations.
- The results challenge the widely held belief that increasing the volume of task-specific training leads to superior neurological outcomes during the early stages of SCI recovery.
Introduction: The Quest for Enhanced Neuroplasticity
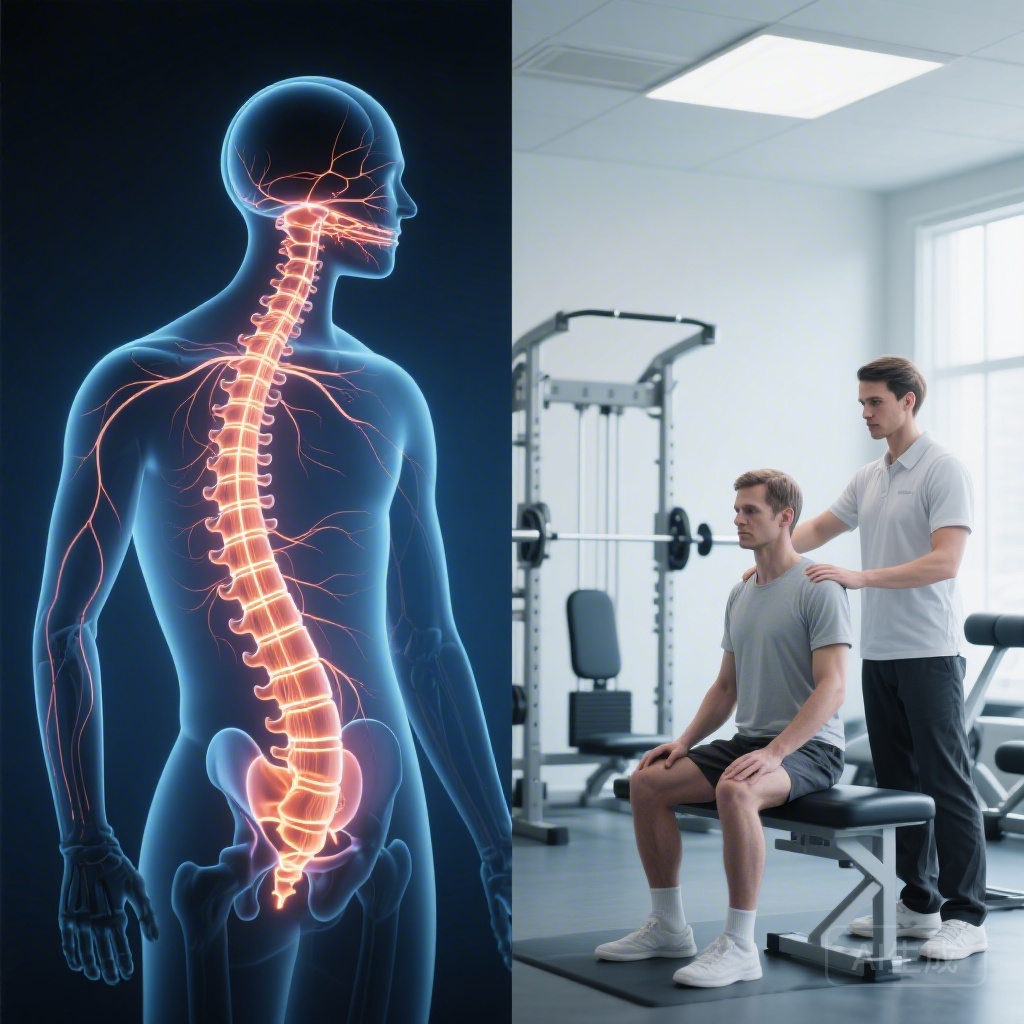
Spinal cord injury (SCI) remains one of the most devastating conditions in clinical medicine, often resulting in permanent loss of motor and sensory function. For decades, the cornerstone of rehabilitation has been the principle of activity-dependent plasticity. This concept suggests that intensive, repetitive, and task-specific training can drive the reorganization of surviving neural circuits, thereby enhancing functional recovery. In clinical practice, this has led to a ‘more is better’ philosophy, where therapists and patients strive for maximum intensity during the early, subacute phase of injury when the nervous system is thought to be most receptive to change.
Despite the biological plausibility of this approach, large-scale, high-quality evidence has been sparse. Most previous studies were either small-scale, non-randomized, or focused on chronic rather than recent injuries. The SCI-MT trial, recently published in The Lancet Neurology, sought to address this evidence gap by rigorously testing whether a massive increase in training volume translates into clinically meaningful improvements in motor function for those with recent injuries.
Study Design: A Global Pragmatic Effort
The SCI-MT trial was a phase 3, pragmatic, randomized, assessor-blinded, superiority trial conducted across 15 specialized hospitals in Australia, Belgium, Italy, the Netherlands, Norway, and the United Kingdom. The pragmatic nature of the trial was intentional, designed to reflect real-world rehabilitation settings while maintaining rigorous scientific controls.
Participants and Randomization
The study enrolled 220 individuals who had sustained a spinal cord injury within the preceding 10 weeks. Eligible participants were required to have some preserved motor function below the level of the lesion (incomplete injury) and be currently receiving inpatient rehabilitation. Participants were randomly assigned (1:1) to either a ‘usual care’ control group (n=111) or an ‘intervention’ group (n=109).
The Intervention Protocol
The intervention was substantial. Participants in the intervention group received their standard usual care plus an additional 12 hours per week of intensive task-specific training for 10 weeks. This training specifically targeted voluntary motor function at and below the level of the lesion and was supplemented with strength training. Task-specific activities included exercises like reach-and-grasp tasks, standing, or gait training, tailored to the individual’s level of injury. The control group received usual inpatient rehabilitation care provided by a multidisciplinary team, which already included physiotherapy and occupational therapy at standard institutional volumes.
Key Findings: A Neutral Outcome for Motor Recovery
The primary endpoint of the trial was the Total Motor Score of the International Standards for the Neurological Classification of SCI (ISNCSCI) at 10 weeks, which ranges from 0 to 100 points. Secondary outcomes included measures of functional independence and quality of life.
Primary Outcome Analysis
At the 10-week mark, data were available for 98% of the participants. The results were strikingly similar between the two groups. The mean Total Motor Score was 78.76 (SD 17.34) in the control group and 78.36 (SD 17.00) in the intervention group. The mean between-group difference was 0.93 points (95% CI -1.63 to 3.48; p=0.48). This statistical result indicates no significant benefit from the additional 120 hours of intensive training provided over the 10-week period.
Secondary Outcomes and Subgroup Analysis
The neutral findings extended to the secondary outcomes as well. There were no significant differences in upper limb motor scores, lower limb motor scores, or functional measures. Subgroup analyses, which looked at factors such as the level of injury (cervical vs. thoracic) and the severity of the injury, also failed to identify a specific cohort that benefited more from the intensive intervention.
Safety and Adverse Events
Safety monitoring revealed four serious adverse events during the study period. Three occurred in the intervention group and one in the control group. Notably, there were two deaths in the intervention group. While these events were scrutinized by the trial’s safety committee, the findings highlight the inherent fragility of patients in the subacute phase of SCI and the importance of balancing intensive physical demands with medical stability.
Expert Commentary: Why Did Intensity Fail to Deliver?
The results of the SCI-MT trial are likely to be met with surprise by many in the rehabilitation community. However, several factors may explain why the intensive training did not yield the expected results.
The ‘Usual Care’ Ceiling
One primary explanation is the high quality of ‘usual care’ in the participating countries. Unlike many previous studies conducted in settings with limited resources, the hospitals in this trial provided robust, multidisciplinary rehabilitation as a standard. It is possible that the standard volume of therapy already maximizes the biological potential for recovery in the first few months post-injury. If the ‘usual care’ group is already reaching a plateau of activity-dependent plasticity, adding more hours may yield diminishing returns.
Biological Constraints of Recent Injury
In the first 10 weeks following a spinal cord injury, the nervous system is undergoing significant inflammatory and metabolic changes. It is possible that during this subacute phase, the capacity for reorganization is limited by biological factors that cannot be overcome by sheer volume of exercise. There may be a ‘biological speed limit’ to axonal sprouting and synaptic remodeling that cannot be accelerated beyond a certain point.
Task Specificity vs. General Strength
The trial combined task-specific training with strength training. While both are standard components of rehab, the heterogeneity of SCI means that what is ‘task-specific’ for one patient may not be for another. The pragmatic design, while excellent for generalizability, might have diluted the effect size that could be seen in more narrowly defined, high-tech interventions like robotic-assisted gait training or targeted electrical stimulation.
Clinical Implications and Future Directions
The findings of this Phase 3 trial have significant implications for health policy and resource allocation. Intensive rehabilitation is expensive, labor-intensive, and demanding for patients. If 12 extra hours of training per week do not result in better motor outcomes, healthcare systems may need to reconsider how they distribute rehabilitation resources.
However, this study should not be interpreted as a reason to reduce rehabilitation standards. Instead, it suggests that rather than simply increasing the *quantity* of training, future research should focus on the *quality* and *timing* of interventions. This might include exploring biological adjuncts—such as stem cell therapies or neuromodulation—that could ‘prime’ the spinal cord to be more responsive to the training already being provided.
Conclusion
The SCI-MT trial provides high-level evidence that intensive task-specific training, when added to high-quality standard inpatient care, does not improve motor recovery in the early stages of spinal cord injury. While disappointing for those hoping for a simple ‘dose-response’ relationship in neurorehabilitation, these results provide a crucial reality check. They emphasize the need for continued innovation in regenerative medicine and more sophisticated approaches to neuroplasticity that go beyond simply increasing the hours spent in the gym.
Funding and Trial Registration
This trial was funded by the New South Wales Ministry of Health, the University of Sydney, and Wings for Life. It is registered with the Australian New Zealand Clinical Trials Registry (ACTRN12621000091808; universal trial number: U1111-1264-1689).
References
1. Glinsky JV, et al. Safety and efficacy of intensive task-specific training in people with recent spinal cord injury: a phase 3, pragmatic, randomised, assessor-blinded, superiority trial. The Lancet Neurology. 2026;25(3):234-244. PMID: 41722590.
2. Harvey LA, et al. Does intensive training improve motor recovery in people with spinal cord injury? A systematic review. Spinal Cord. 2017;55(9):800-811.
3. Dietz V, Fouad K. Restoration of sensorimotor functions after spinal cord injury. Neural Plasticity. 2014;2014:1-12.